Researchers Suggest New Treatment Guidelines For Treating Pulmonary Hypertension Due to Sickle Cell Disease
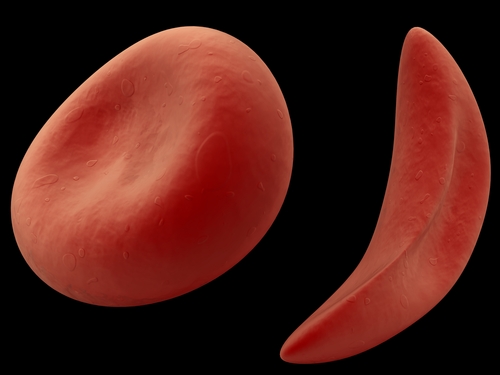
 Sickle Cell disease (SCD) is one of the most prevalent genetic diseases worldwide. It is a type of anemia characterized by the hemoglobin variant hemoglobin S (HbS), which causes rigidity in red cells and “sickling.” This sickling changes their shape, resulting in a number of life-long complications for patients with the disease.
Sickle Cell disease (SCD) is one of the most prevalent genetic diseases worldwide. It is a type of anemia characterized by the hemoglobin variant hemoglobin S (HbS), which causes rigidity in red cells and “sickling.” This sickling changes their shape, resulting in a number of life-long complications for patients with the disease.
An increase of the red blood breakdown within the blood vessels cause inflammation and a constriction of the small arteries of the lungs, leading to pulmonary hypertension (PH). The progression of PH has been found to develop in 30% of adult patients with SCD.
[adrotate group=”4″]
A research group leader by Dr. Elizabeth Kilings from Boston University produced evidence-based management recommendations for adult patients who suffer from pulmonary hypertension complications due to SCD. Dr. Kilings’ research, which involved the consultation of a multidisciplinary committee, recommended that, “decision making should be guided by stratification of mortality risk.” The study went on to suggest that, “for patients with increased mortality risk (defined as tricuspid regurgitant velocity [TRV] ≥2.5 m/second; serum N-terminal pro-brain natriuretic peptide [NT-pro-BNP] ≥160 pg/mL; or right heart catheterization [RHC]-confirmed pulmonary hypertension), hydroxyurea was strongly recommended as first-line therapy, and chronic transfusions were weakly recommended as an alternative therapy.” However, the authors of the study strongly recommended that doctors avoid pulmonary arterial hypertension therapy for SCD patients that only presented with “elevated TRV alone, elevated serum NT-pro-BNP alone, and for those with RHC-confirmed pulmonary hypertension with elevated pulmonary capillary wedge pressure and low pulmonary vascular resistance.”
The report also noted that, “there was a weak recommendation for prostanoid or endothelia receptor antagonist therapy, and a strong recommendation against phosphodeisterase-5 inhibitor therapy for select patients with SCD with RHC-confirmed pulmonary hypertension with increased pulmonary vascular resistance and normal pulmonary capillary wedge pressure.”
[adrotate group=”3″]
In and of itself, Sickle Cell disease presents with a wide range of complications that, when compounded with the onset of Pulmonary Hypertension, can make it exceedingly difficult to effectively treat the patient. However, with these newly suggested guidelines, medical practitioners will be in a better position to offer targeted therapy for PH while still continuing to address the symptoms and health complications of SCD as well.







