New Procedure Successfully Treats CTEPH Patient at Northwestern Hospital in Illinois
A new procedure, performed at Northwestern Memorial Hospital in Illinois, successfully treated a patient with pulmonary hypertension (PH) caused by blood clots formed in the lung vessels, a condition referred to as chronic thromboembolic pulmonary hypertension (CTEPH).
This new treatment is less invasive than the surgical removal of the clots — or pulmonary endarterectomy (PEA)— which is usually the treatment of choice, offering an alternative option for CTEPH patients who cannot undergo surgery.
This was the first time the procedure was performed in Illinois, and Northwestern now joins the ranks of only a handful of centers across the U.S. that offer it.
According to a press release, the procedure — called balloon pulmonary angioplasty (BPA) — was pioneered in patient Sherry Seals who had chest pain and shortness of breath that would not go away, ultimately leading to a diagnosis of CTEPH.
She had several blood clots spread through her lung vessels, which were causing high blood pressure. The clots would not dissolve with medication, and there were too many and they were too spread out to be removed by PEA.
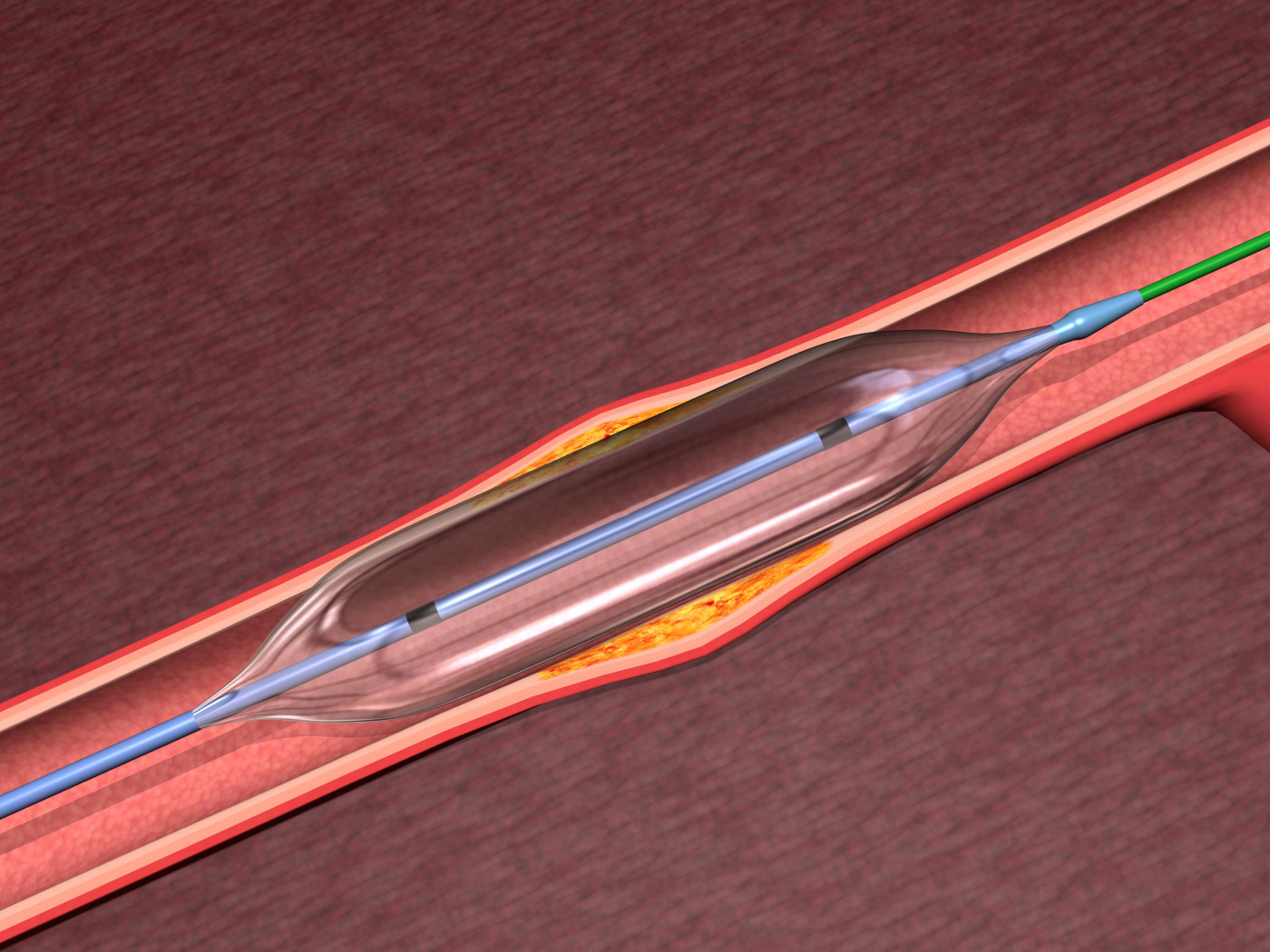
But Seals was eligible for BPA, which is similar to coronary angioplasty, a common procedure where a balloon is used to widen blocked or narrowed heart arteries.
Ask questions and share your knowledge of PH in our forums.
Daniel J. Schimmel Jr., MD, a cardiologist at Northwestern and professor at the Feinberg School of Medicine, performed the procedure. Schimmel had been training on the technique with the Japanese physician who perfected it.
The treatment involves sending a narrow tube through the femoral vein in the upper leg while the patient is under local anesthetic. The tube transports a tiny balloon (ranging from 1.5 to 6 mm in diameter) through the chambers of the heart into the narrowed lung arteries.
Once there, the balloon is inflated to widen arteries to their normal size, restoring blood flow in the lungs and reducing high pressure to levels closer to normal.
During the procedure, contrast dye and X-rays are used to identify the blockage sites in real time.
As opposed to conventional angioplasty, BPA breaks fibrotic tissue and widens blood vessels without affecting inner vessel layers, and repeat sessions are generally required. Treatments are performed with various sizes of balloons.
“For the first two procedures, the goal is not to expand the artery to normal, but to get the lung tissue used to seeing blood flow again,” Schimmel said in the release. “If the lung tissue sees too much flow too fast, it can create injury. Follow-up procedures are meant to restore the artery to its normal size and return pressure in the lungs to normal. Patients often are not back to normal but start to feel improvement after the second procedure.”
In total, Seals has had five BPA interventions, but she had already started to notice improvements right after the second treatment.
“I didn’t care if this was a new procedure, I just wanted to feel good again,” Seals said. “After each procedure I was breathing a little better.”
Now, she says, she can walk longer without losing her breath. “I can flip through the stairs, jump down, walk up, do it three times in a row if I was allowed to,” said Seals, who lives on the second floor of her building. “I am breathing so much better.”
In Illinois, Northwestern is now the only hospital offering BPA, along with PEA and pulmonary vasodilator medications, as treatment options for CTEPH.
“Some patients respond well to medication, and there are some new investigational drugs being tested. Other patients are candidates for BPA, but others may need an operation. BPA isn’t the right treatment for everyone, but in some cases it can be a game changer,” Schimmel said.
“As our experience has grown, we are beginning to consider combining all three of these approaches in a patient to personalize the treatments for the best outcomes,” said Stuart Rich, MD, director of the Pulmonary Vascular Disease Program at Northwestern and a professor at Feinberg.
Northwestern Memorial Hospital is ranked first in the U.S. for heart failure survival, and it is accredited by the Pulmonary Hypertension Association as a Comprehensive Care Center, the highest recognition for medical centers treating PH.







