My Recent CPAP Use Has Triggered Traumatic Memories
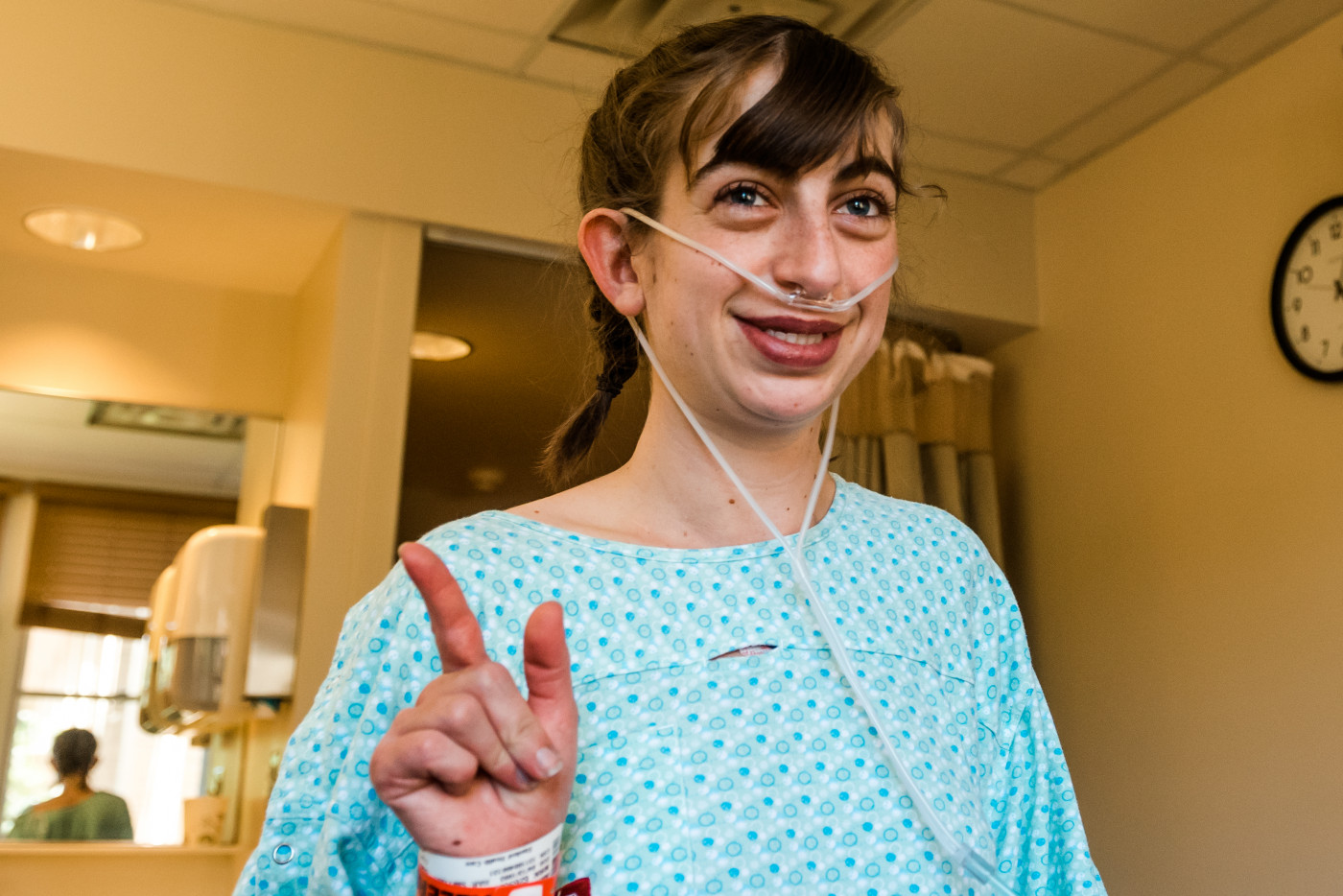
Kathleen wearing oxygen hours before operation. (Photo by Monica Sheffer)
For 16 years I slept with supplemental oxygen delivered through a nasal cannula. Prone to desaturation at night, I blasted two liters of concentrated oxygen through my nose every minute in an attempt to keep my bloodstream’s amount of oxygen at a safe level.
When my pulmonary hypertension progressed, I transitioned to using supplemental oxygen around the clock. Tethered to both an oxygen concentrator and infusion pump administering intravenous medication, I felt constrained; often physically tangled up in tubes.
After my surgery, I got off oxygen as soon as possible. I never looked back. One of the best perks of my heart-lung transplant has been freedom from all machines. This is a whole new way of living for me. It took several months for me to stop reaching for my pump whenever I stand.
During my first bronchoscopy, a procedure to diagnose infection and rejection in my transplanted lungs, my anxiety spiked when the anesthesiologist put an oxygen cannula on me. “I haven’t been on any oxygen for TWO MONTHS!” I protested. “My saturation is always 100!” He didn’t care.
Though I’ve gotten used to wearing oxygen during procedures, my fear of returning to a life attached to machines lingers.
Earlier this month, I was diagnosed with severe obstructive sleep apnea. Last week I started using a continuous positive airway pressure (CPAP) machine at night. In an overnight sleep study, the machine effectively kept my airways open through its application of continuous air pressure. My doctor showed me graphs demonstrating the difference it made. “You need help,” were his exact words, admitting his surprise at the severity of my apnea, given my age. Add that to the list of reasons I do not feel 25 — among my 56-year-old heart and lungs, my love for Grape Nuts, and early bedtimes.
Ask questions and share your knowledge of PH in our forums.
The first night was miserable. I kept waking up in fear that I was wearing an oxygen mask, and that I was sick again. Even though I know many of my friends and readers endure so much more on a nightly basis, making this a part of my nightly routine brings me deep sadness.
The CPAP highlights one of my greatest fears: that my new, hard-fought health is fleeting, that I will again require life-sustaining machines. Starting CPAP therapy feels like a step backward after freeing myself from tubing. Internally I feel like my six-year-old self, battling against the nurses and my parents who insisted I needed to wear the oxygen cannula. I want to cry and scream and tear it off my face.
Logically, though, I know it’s a step in the right direction. The hope is that it will improve my sleep and give me even more energy on a daily basis.
Have you been diagnosed with sleep apnea? Share your experience in our forums.
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, BioNews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.









Comments
srivari
Good One
srivari
Informative one