Pulmonary Arterial Hypertension Study Targets Abnormal Smooth Muscle Cell Growth
 A new study, entitled “The Sphingosine Kinase 1 / Sphingosine-1-Phosphate Pathway in Pulmonary Arterial Hypertension” conducted at University of Illinois’s College of Medicine, at Chicago, published in the American Journal of Respiratory and Critical Care Medicine, by Dr. Jiwang Chen, research assistant professor of critical care medicine, sleep and allergy, and his colleagues, identify two new potential therapeutic targets for the treatment of pulmonary arterial hypertension (PAH), a fatal disease characterized by high blood pressure in the lungs. This study was conducted by the research groups of Dr. Roberto Machado, associate professor of pulmonary, critical care, sleep and allergy, and Dr. Viswanathan Natarajan, professor of pharmacology, both of whom served as the senior authors on this paper.
A new study, entitled “The Sphingosine Kinase 1 / Sphingosine-1-Phosphate Pathway in Pulmonary Arterial Hypertension” conducted at University of Illinois’s College of Medicine, at Chicago, published in the American Journal of Respiratory and Critical Care Medicine, by Dr. Jiwang Chen, research assistant professor of critical care medicine, sleep and allergy, and his colleagues, identify two new potential therapeutic targets for the treatment of pulmonary arterial hypertension (PAH), a fatal disease characterized by high blood pressure in the lungs. This study was conducted by the research groups of Dr. Roberto Machado, associate professor of pulmonary, critical care, sleep and allergy, and Dr. Viswanathan Natarajan, professor of pharmacology, both of whom served as the senior authors on this paper.
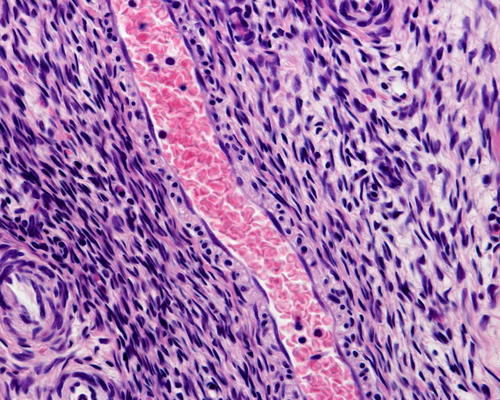
PAH is characterized by chronic increase in pulmonary arterial (PA) resistance and pressure. One of the main factors that could induce the increased pulmonary arterial pressure is the narrowing of the pulmonary blood vessels, which could be due to an abnormal proliferation of cells within the walls of the blood vessels, predominantly the smooth muscle cells of the pulmonary artery. The early symptoms of PAH include shortness of breath and exercise intolerance. As the disease progresses, patients may require oxygen supplementation and lung transplantation. The patients can develop heart failure, a major cause of death in the disease. PAH may also result from respiratory and cardiac diseases like scleroderma, congenital heart disease, and liver disease, and overall has a poor prognosis.
[adrotate group=”4″]
Dr. Chen and colleagues decided to investigate the molecular mechanisms behind the abnormal proliferation of smooth muscle cells in the pulmonary artery and discovered two ways that the proliferation could be inhibited. “The characteristic proliferation of cells that line the blood vessels in pulmonary hypertension is similar to the abnormal growth and reproduction of cells that form cancerous tumors,” said Dr. Chen. It is known that an enzyme, sphingosine kinase 1, which produces a signaling molecule called sphingosine-1-phosphate (S1P), had been linked to the abnormal growth of cells in cancer, including lung cancer. “We wanted to see if sphingosine kinase 1 and S1P were involved in the development of pulmonary arterial hypertension,” added Dr. Chen. Therefore, the researchers analyzed samples of lung tissue from patients and found that patients with pulmonary arterial hypertension had significantly increased levels of both the enzyme sphingosine kinase 1 and, its product, sphingosine-1-phosphate (S1P). They found similar increased levels of both molecules in mouse and rat models of pulmonary hypertension.
[adrotate group=”3″]
During the study, researchers used a rodent model deficient for the gene of sphingosine kinase 1 and observed that these mice were less susceptible to develop pulmonary hypertension than normal mice when exposed to the low-oxygen conditions used to induce the disease in the laboratory. The researchers used drugs that either suppress production of sphingosine kinase 1 or block the signaling of S1P through its receptors on smooth muscle cells, and inhibited, in low-oxygen conditions, the development of pulmonary hypertension in mice. Moreover, they showed that over-production of sphingosine kinase 1 and S1P promote the proliferation of pulmonary artery smooth muscle cells in mice.
“Our results yield two new potential targets for the development of drugs to treat or prevent the progression of pulmonary arterial hypertension,” said Dr. Chen. “By blocking the binding site for S1P or suppressing the production of S1P, like we did in our experimental rodent model over-production of sphingosine kinase 1 and S1P promote the proliferation of pulmonary artery smooth muscle cells, we can reduce the proliferation of pulmonary artery smooth muscle cells, which is a major contributor to pulmonary hypertension,” concluded Dr. Chen.







