Novel Surgical CTEPH Treatment Approach Cures Disease
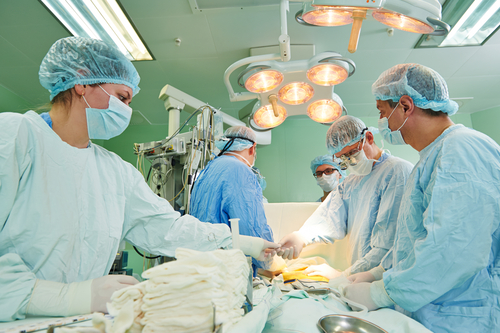
 Vanderbilt Heart & Vascular Institute (VHVI) is offering a novel and specialized surgical approach for treating patients suffering from chronic thromboembolic pulmonary hypertension (CTEPH), a form of pulmonary hypertension (PH) that can cause breathing difficulties, acute pulmonary embolism, or blood clots in the lung. Even though the condition is rare and often misdiagnosed, several efforts have been made to support patients, including the creation of the first annual CTEPH Awareness Day by the Pulmonary Hypertension Association, which was celebrated on Tuesday, November 18.
Vanderbilt Heart & Vascular Institute (VHVI) is offering a novel and specialized surgical approach for treating patients suffering from chronic thromboembolic pulmonary hypertension (CTEPH), a form of pulmonary hypertension (PH) that can cause breathing difficulties, acute pulmonary embolism, or blood clots in the lung. Even though the condition is rare and often misdiagnosed, several efforts have been made to support patients, including the creation of the first annual CTEPH Awareness Day by the Pulmonary Hypertension Association, which was celebrated on Tuesday, November 18.
Severe cases of CTEPH can be fatal, as some patients are not able to resolve the blood clots normally and form chronic ones, as well as scar tissue and pulmonary artery obstruction, which can lead to strain on the right side of the heart and as a consequence, heart failure. However, the surgical procedure being conducted at VHVI, pulmonary thromboendarterectomy, aims to resolve the problem. However, it is a complex, high-risk operation that is only indicated for a specific type of patient.
[adrotate group=”4″]
“Many of these patients see a doctor who says there is nothing that can be done for them. We’re one of the few medical centers in this part of the country doing this procedure,” said Michael Petracek, M.D., chair of Vanderbilt’s Department of Cardiac Surgery, one of less than ten medical centers in the United States to offer the procedure, during which patients are placed on a heart-lung machine and their body temperature is cooled to 64.4 degrees Fahrenheit so that surgeons are able to open he chest via median sternotomy.
“They have no blood supply to the brain while I go in and take out scar tissue from their lungs. You have a short period of time to do it,” Petracek said. “I do both sides in 20-minute intervals and relieve their pulmonary hypertension in order to get their heart function back to normal.”
The first step into treatment is diagnosing the condition, which is already difficult. The pulmologist at VHVI, Ivan Robbins, M.D., professor of Medicine, commonly sees patients who are experiencing shortness of breath, on oxygen, and who need to rest just after a short distance of walking. However, these symptoms are common in other lung diseases, which can lead to a misdiagnosis of asthma or chronic obstructive pulmonary disease (COPD).
[adrotate group=”3″]
“Usually patients will come with very nondescript symptoms and an echocardiogram, showing evidence of pulmonary hypertension, is often the first clue that a patient has CTEPH,” explained Robbins. “Surgery can be curative and the results can be dramatic. We’ve had people with severe pulmonary hypertension, who, at the conclusion of surgery, have normal or near normal pressures in their lungs. Of all the forms of pulmonary hypertension, CTEPH is the only one that can be cured.”
Even though pulmonary thromboendarterectomy is indicated for CTEPH patients who haven’t yet developed heart failure, the procedure may also be helpful in patients with cardiac dysfunction. “People don’t realize there’s treatment for this type of pulmonary hypertension. This is one that is very curable, but it requires a big operation that not many medical centers do. We’ve got a unique situation at Vanderbilt because we’ve got people here who really understand pulmonary hypertension,” added Petracek, who is currently training other surgeons on pulmonary thromboendarterectomy.







