Staying Healthy While Traveling with Transplanted Organs

Tram in Prague. (Photo by Kathleen Sheffer)
For the first couple months of my recovery from a heart-lung transplant, I had a one-hour radius from the hospital. A woman I met in a waiting room assured me that eventually, I would be able to travel internationally. “They just load you up with antibiotics and you’re good to go,” she said. I remained skeptical.
Twenty months later, I found myself driving a rental car on the left side of a freeway at night in pouring rain. Traveling through Europe last month increased my independence and confidence in my own strength and adaptability. The trip challenged me to adapt to different languages, time zones, currencies, and transportation systems. It would have been an adventure even without the added complication of my compromised immune system and regimented medications.
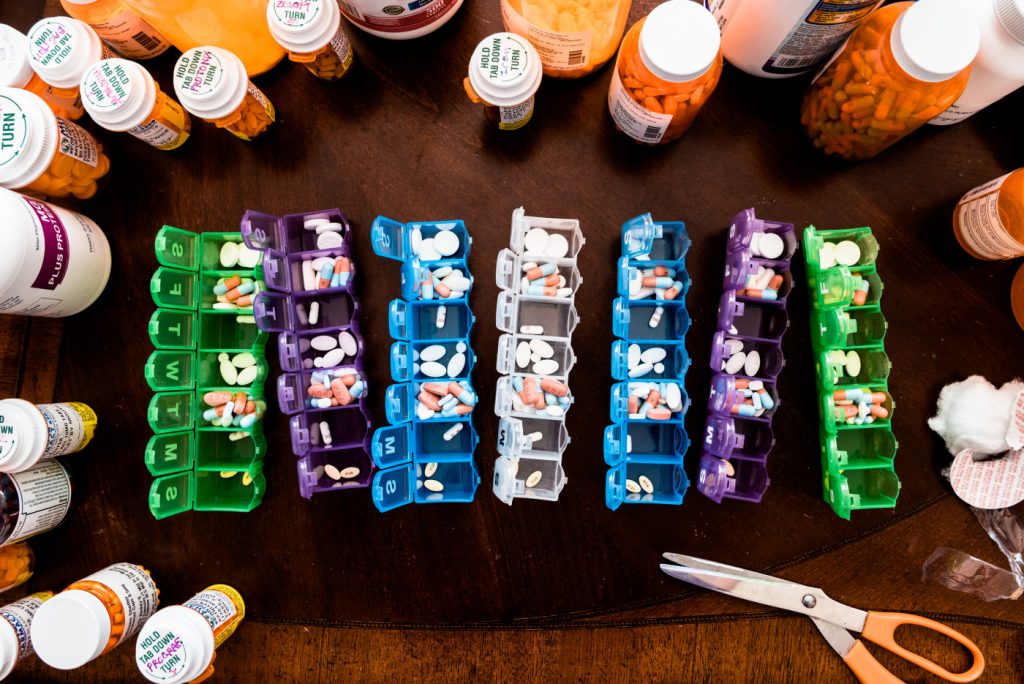
I was over-prepared for the trip. A month and a half supply of medication for 30 days of travel. A stack of Wet Ones packs, protein bars, three N99 masks. Homeopathic cold and flu shortening treatments, and a full course of antibiotics just in case. I made a spreadsheet with an emergency hospital assigned to all eight of the major cities we visited.
But the only emergencies I had were Emergen-C packets stirred into glasses of water before each flight. (I’m just as horrified as you that I wrote that sentence. And left it.) I didn’t get sick and my pulmonary function remained stable. My labs looked good the week I returned, so I didn’t need to adjust any medications.
I proved to myself that I could carry my own suitcase and backpack up staircase after staircase (appreciating the impact of the Americans with Disabilities Act along the way), wear an N99 mask for the duration of a long flight, and avoid illness while traveling.
How did I not get sick during a month of foreign travel on immunosuppressant medications? It wasn’t all luck.
Food safety
Most of the precautions I took revolved around food. First and foremost, I did not share food or beverages with anyone, except the occasional pretzel or mass of sauerkraut, if and only if my sister and I portioned it out before starting to eat. Not exchanging saliva is key to avoiding illness. Yuck – even the word saliva is gross.
Not only are transplant recipients more susceptible to foodborne illnesses, we are more likely to experience a longer period of illness, be hospitalized, or even die, should we contract one. I ate only at restaurants that appeared reputable, checking reviews and health department ratings whenever possible. No street kebab for me. I was especially careful about eating meat, frequently opting for vegetarian options that typically come with fewer food safety issues. Twice I sent food back because the meat was undercooked.
In the United States, restaurants generally serve only pasteurized cheeses, and it’s easy enough to ask a waiter to check with the chef, but it was hard to be sure at restaurants in Europe. I stuck to hard cheeses, avoiding ingredients like feta and blue cheese, which are often unpasteurized.
Hydration
I bought a lot of pricey glass bottles of water at restaurants in Germany. Staying hydrated with clean water (none of those questionably clean pitchers filled with questionably clean ice) was well worth it. Transplant medications take a toll on the kidneys, so drinking plenty of water is always critical for me.
Rest
My sister and I are two hip young women in our early 20s … who value our sleep. I don’t think we were ever up past midnight the entire trip. When I traveled with pulmonary hypertension, jet lag took a greater toll on me than on my companions. Fortunately, I experienced very little fatigue on this trip. We had jam-packed days with hikes and trips to rock climbing gyms combined with museum tours and urban exploration. I was thrilled to be able to get through each day without napping, go to bed early, sleep through the night, and wake up rested — all without supplemental oxygen.
Mask on
I wore my Vogmask N99 mask in crowded areas: on buses, trains, and planes, in gyms, museum elevators … wherever I felt like I might breathe the air another human coughed out. I’m constantly redefining my comfort level, wearing my mask whenever my anxiety about infection outweighs my enjoyment of mask-free breathing. Lots of transplant patients never wear a mask, but it gives me peace of mind and so far has proven effective.
As much as I wanted to go on this epic trip, I feared it was too great a risk to take. Unwilling to trade my newly stable health status for a trip to Europe, I was deeply worried about getting sick or rejecting my transplants while abroad. As with all the risks I take (see: rock climbing), I approached it with preparation and caution. I did it as safely as I knew how. It paid off: Now I can write about staying healthy while traveling!
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.












Kaye Norlin
Thanks for that, Kathleen. I followed your trip on Facebook and lived vicariously through your adventures. I am planning on going to Europe in October 2019 if I get the approval from my transplant team. I am excited to be planning this trip post-transplant; my last trip there with my husband and kids was with PAH and was difficult. There is town in Italy that has an approach with a 40 degree incline to reach it- no cars- and I will make it there.
Kathleen Sheffer
Love this! That's a great goal, and totally doable since you are rocking your transplant!
Boomer Bozarth
Thanks again for your story. I'm still a little scared about going different places other than around my neighborhood or county. I had PH for 18 years. After reading your story I guess it's time to get myself in gear an put my big boy pants on and start living again. It will be 2 years since my double lung transplant this 4th of July. Thank you again
Kathleen Sheffer
Thank you for your comment, Boomer! I would love to hear more of your story (maybe in our Forums??) because it sounds so similar to mine. I was transplanted on 7/1/16, just three days ahead of you, and had been diagnosed with PH for 16 years. Totally understandable that you are scared - so was I! But we gain confidence by taking these risks and proving to ourselves we can do them safely. Can't wait to hear about your adventure!
Kaye Norlin
Yay!!! Go for it!!! Celebrate your second life!!!