Pulmonary Hypertension, Other Lung Disease Research To Benefit from Cutting-Edge Lung Imaging Innovation
Written by |
 The U.K.’s Chancellor of the Exchequer, George Osborne, has announced that the University of Sheffield will be awarded £7.5 million to expand development of its world-leading clinical lung imaging research — technology that may lead to significant advances in treating a wide range of pulmonary disease, including Pulmonary Hypertension.
The U.K.’s Chancellor of the Exchequer, George Osborne, has announced that the University of Sheffield will be awarded £7.5 million to expand development of its world-leading clinical lung imaging research — technology that may lead to significant advances in treating a wide range of pulmonary disease, including Pulmonary Hypertension.
The Academic Unit of Radiology in the University of Sheffield’s Department of Cardiovascular Science, is one of several key research groups contributing to the recently established Insigneo Institute for in silica Medicine. The multi-disciplinary institute involving over 80 academics and clinicians is a collaborative initiative between the University of Sheffield and Sheffield Teaching Hospitals National Health Services (NHS) Foundation Trust. Members collaborate to develop computer simulations of the human body and its disease processes that can be used directly in clinical practice to improve diagnosis and treatment.
This initiative is probably the most sophisticated application of computing technology in healthcare. U. Sheffield has become the UK’s main center for this work, and is internationally leading in research and development of technology for clinical lung imaging with hyper polarized gases and proton MRI, which provide very detailed images of patients lungs, without relying on X-rays’ radiation.
[adrotate group=”4″]
Using these state-of-the-art techniques developed in Sheffield, by the Pulmonary, Lung and Respiratory Imaging Sheffield (POLARIS) project, led by Professor Jim Wild, the team creates functional images of the lungs in patients affected by conditions such as smoking, cystic fibrosis, emphysema, pulmonary hypertension and asthma. Collaborating with clinicians in Sheffield and across the UK they have led the way in translating these techniques in to the clinic.
The POLARIS group have pioneered use of hyperpolarized gases and proton lung MRI for the evaluation of regional lung response to therapeutics in Asthma, CF, COPD and PH. The techniques are free from ionizing radiation and highly sensitive to changes in lung function and as such are ideally suited for therapy assessment. Collaborations are in place with Novartis and GSK in this area and we have a track record in delivering commercial contract work with pharma using clinical lung imaging as outcome measures in trials.
Clinical Imaging Research in Respiratory Diseases
Sheffield performed the first clinical studies in the UK with both hyperpolarized 3He and 129Xe gas MRI. In collaboration with pulmonary clinicians from Sheffield and elsewhere in the UK (Manchester, Leicester) and Europe (Rotterdam, Dublin), the researchers have demonstrated the clinical role of these MRI methods in different lung diseases:
• Emphysema – POLARIS were the first group in the world to demonstrate alveolar destruction and ventilation inhomogeneity in healthy smokers preceding changes in clinical gold standards spirometry and CT. In patients with COPD they have demonstrated collateral ventilation pathways by measuring gas wash-in.
[adrotate group=”3″]
• Cystic Fibrosis – POLARIS have shown obstructive changes in lung ventilation in adults and children with sensitivity greater than X ray and equal to CT. The non-ionizing nature of lung MRI makes it ideal for longitudinal radiological follow-up of this patient group and POLARIS researchers were the first to demonstrate the sensitivity to changes in regional lung function with therapy in patients from the Sheffield Children’s Hospital.
MRI of Pulmonary Vascular Disease
In pulmonary vascular disease, POLARIS researchers have changed radiological practice with new imaging technology uptake for patient benefit, which is now part of the NHS funded clinical workup for over 25 percent of the UK population of adult patients with Pulmonary Hypertension. The Sheffield Pulmonary Vascular Unit (the largest referral clinic in the UK), now routinely scan patients with lung MRI protocols developed by the POLARIS group — the largest pulmonary vascular MRI cohort in the world. The MRI lung perfusion scans and MR angiograms developed have replaced nuclear medicine V/Q for screening for chronic thrombo-embolic pulmonary hypertension and X-ray pulmonary angiogram scans to plan for pulmonary endarterectomy (modalities currently used elsewhere in the UK). POLARIS techniques provide superior image quality while saving patients an unnecessary radiation dose (1-2 and 6 mSv respectively) and an invasive catheter procedure with associated morbidity (serious adverse events 1% and mortality <0.1%). Other sites in the UK NHS e.g. Papworth the National Referral centre for pulmonary enarterectomy and Edinburgh have adopted our MR protocols for pulmonary vascular disease.
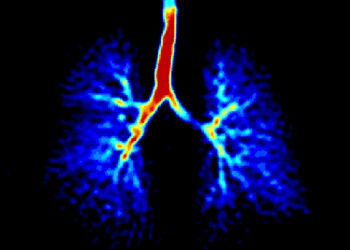
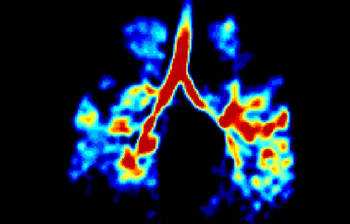
A U. Sheffield release notes that the technique of hyperpolarized gas MRI involves a person inhaling small amounts of noble gases (Helium-3 and Xenon-129), which are then imaged inside an MRI scanner. The gases are hyperpolarized using high power lasers by a process called optical pumping. The group has developed specialized gas laser polarizers and custom MRI scanner hardware which provide high-resolution images that are not currently available with conventional methods.
The innovative imaging technology illuminates lung function and helps clinicians identify early signs of lung disease, for example earlier diagnosis of emphysema and smoking related damage, as well as other lung conditions and diseases such as pulmonary fibrosis, asthma, pulmonary hypertension, and cystic fibrosis.
However, several technical barriers, such as ease of polarization of the gases used and the additional hardware required for the MRI scanners, still need to be overcome before this technology can become a more routinely used clinical method across the UK.
The new grant, which is made up of £6.5 million from the Medical Research Council and a further £1 million from the British Heart Foundation, will allow the expansion of the ground-breaking image acquisition and processing facilities in Sheffield, in turn making the UK the leading nation in this important area of diagnostic pulmonary medicine.
The award is part of a £230 million grant for technologies to revolutionize research into disease led by the Medical Research Council (MRC). The money will be invested in a range of revolutionary technologies aimed at identifying the causes of diseases such as cancer and dementia, and dramatically speeding up diagnosis and treatment. The state-of-the-art technologies will be used to find out how differences in the cellular and molecular make-up of people affect how they respond to diseases and to treatment.
Jim Wild, Professor of Magnetic Resonance Physics and NIHR Research Professor in Pulmonary Imaging, says: “This grant will allow continued research into MRI scanner hardware and image acquisition methods and their clinical translation ensuring Sheffield and the UK leads in this important area of diagnostic pulmonary medicine.
“The new image processing laboratory will allow us to process large volumes of digital imaging data for phenotyping pulmonary diseases together with computational modeling approaches being pioneered in the University’s Insigneo Institute for in silico medicine which brings together engineers, scientists and clinicians from across the University of Sheffield, and Sheffield Teaching Hospitals NHS Foundation Trust.”
For more information about POLARIS please visit:
https://www.shef.ac.uk/polaris
Insigneo Institute for in silico Medicine
https://www.insigneo.org
With almost 26,000 of the brightest students from around 120 countries, learning alongside over 1,200 of the best academics from across the globe, the University of Sheffield is one of the worlds leading universities.
A member of the UKs prestigious Russell Group of leading research-led institutions, Sheffield offers world-class teaching and research excellence across a wide range of disciplines.
Unified by the power of discovery and understanding, staff and students at the university are committed to finding new ways to transform the world we live in.
In 2014, the University of Sheffield was voted number one university in the UK for Student Satisfaction by Times Higher Education and in the last decade has won four Queens Anniversary Prizes in recognition of the outstanding contribution to the United Kingdoms intellectual, economic, cultural and social life.
Sheffield has five Nobel Prize winners among former staff and students and its alumni go on to hold positions of great responsibility and influence all over the world, making significant contributions in their chosen fields.
Global research partners and clients include Boeing, Rolls-Royce, Unilever, AstraZeneca, Glaxo SmithKline, Siemens and Airbus, as well as many UK and overseas government agencies and charitable foundations.
The Academic Unit of Radiology (AuR) at Sheffield has seven senior academics (three academic radiologists and four MR physicists), one clinical research fellow (post CCT) and twelve Research assistants/PhD students. There are four MR scanners, each with ring-fenced research time, and the research in the section is based around that technique. They recently installed a state of the art Philips Ingenia wide bore 3T scanner funded by the Wellcome Trust. Research grant income for the preceding five years exceeds £5m and commercial income was over £5m.
The AuR is situated within the Clinical Radiology Department on the Hallamshire Hospital site. The department routinely publishes 30-35 papers per year in peer-reviewed journals.
The AuR has research partnerships with two major MR manufacturers (Philips Medical Systems and General Electric Health Care) and has an active research program which is progressing on a variety of fronts, including:
Hyperpolarized Gas MRI Of Lungs
Academic Unit of Radiology researchers have been working on novel inhaled contrast enhancement mechanisms for imaging lung ventilation using the signal of inhaled hyperpolarized (HP) noble gases. The images produced are supplying clinicians with anatomical and functional information of the pulmonary system that has previously been unattainable. The first clinical studies in the UK to use inhaled hyperpolarized 3He MRI have taken place at the University and much technological development work has been done to establish the group as a world centre in this emergent branch of diagnostic imaging.
The AuR has developed strong collaborations in obstetrics and is leading a multicenter HTA trial of in utero MR imaging; Sheffield is an internationally recognized centre for multinuclear (3He, 129Xe and 13C) MR imaging and collaborates with Europe’s largest clinic for pulmonary hypertension based in Sheffield; we undertake fMRI with the academic departments of Psychology and Psychiatry; more recently we have developed collaborations with the NIHR metabolic bone BRU including design of novel bone turnover MR contrast agents; we have recently be granted a 3m+ Welcome Trust grant is to develop 3TMR scanners for neonatal ITU use with GE medical systems. The unit is firmly embedded in a new University Institute, Insigneo, which has internationally recognized modeling and image processing groups that compliment the medical imaging undertaken in the unit and there are numerous opportunities for collaboration. Insigneo is addressing such areas as stratified and personalized medicine and engineering for life.
Previous AuR ACFs have collectively generated over 20 publications whilst in post. The unit has an established track record for developing and creating academic radiologists. Two NIHR academic clinical lecturers are currently in post as HEFCE funded senior lecturers and another is in a senior academic position at the Sick Children’s Hospital, Toronto.
The Academic Unit of Radiology at the University of Sheffield currently operates four MR scanners at different sites across Sheffield; two based at the Royal Hallamshire Hospital (1.5T and 3T), Sheffield Children’s Hospital (1.5T) and a small bore 0.2T system based at the Jessop Wing of the Royal Hallamshire Hospital.
Sources:
University of Sheffield
Office of the U.K. Chancellor of the Exchequer
Imag Credits:
University of Sheffield
Office of the U.K. Chancellor of the Exchequer