Switching to Inhaled Treprostinil Combo Safe, Effective in Stable PAH Patients, Study Suggests
Written by |
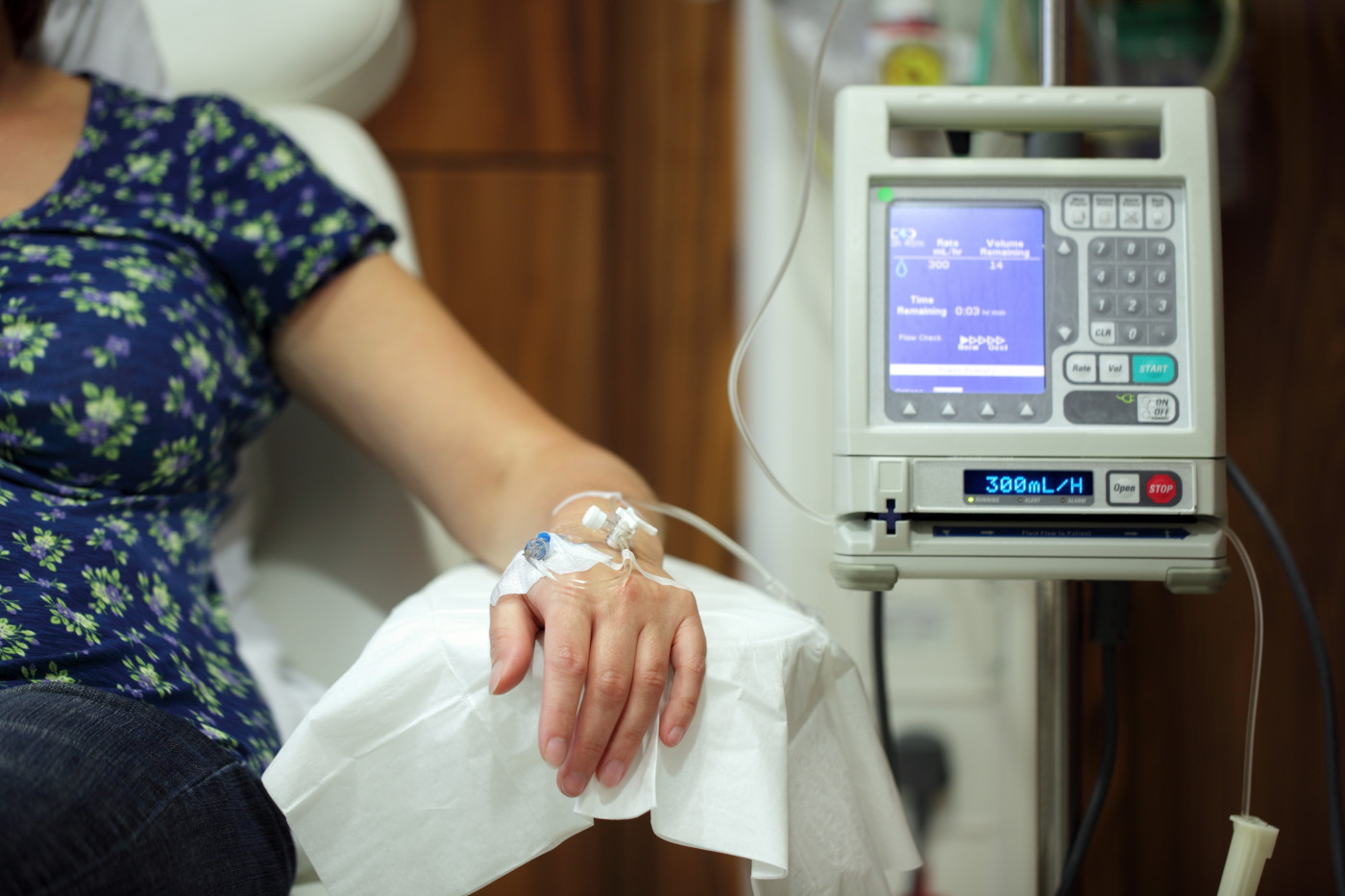
Switching from injectable treprostinil or epoprostenol to a combination therapy including inhaled treprostinil appears to be safe, well tolerated, and effective for a select group of patients with clinically stable pulmonary arterial hypertension (PAH), a study suggests.
The study, “Ambulatory Transition from Parenteral Prostanoid to Inhaled Treprostinil in Patients with Pulmonary Arterial Hypertension,” was published in the journal Lung.
Treprostinil (sold as Remodulin by United Therapeutics) and epoprostenol (sold as Flolan by GSK and Veletri by Actelion Pharmaceuticals) are two prostanoid agents used in the treatment of PAH.
Prostanoid agents are manmade mimics of the hormone prostacyclin that work by activating signaling pathways that cause blood vessels to relax and widen (vasodilation), improving blood flow. These compounds also prevent platelets from clumping and blocking arteries.
Although effective, continuous administration of these agents through under-the-skin injections (subcutaneous injections) or directly into the bloodstream (intravenous infusions) may be hampered by access difficulties, need for daily preparation, and infusion pump management.
In addition, treatment may lead to infusion-related side effects, including infections, skin irritation, and pain. It can also be costly, placing a financial burden on patients.
Because injectable agents are considered more efficacious, patients with high-risk disease profiles are usually advised to include at least one of these compounds in their maintenance treatment regimen.
However, patients at low or intermediate risk and with less severe symptoms may benefit more from treatment with inhaled or oral formulations, which are potentially safer as they avoid most side effects and complications associated with injectables.
It hasn’t been established how to select those who are more likely to benefit from switching therapy formulations, or whether it’s best to do so in a medical office or at home.
Researchers from the University of Chicago reviewed the medical records of 16 PAH patients who transitioned from an intravenous or subcutaneous treatment regimen with prostanoids to a non-injectable, combination treatment that included inhaled treprostinil (sold as Tyvaso by United Therapeutics) administered at home.
All were clinically stable, and had favorable risk profiles. Most of them (81.25%) had a WHO functional classification of I or II, meaning they didn’t experience symptoms while exercising or at rest, but might feel uncomfortable and out of breath with ordinary activities such as climbing stairs or shopping.
Of the 16 patients analyzed, nine were being treated with intravenous treprostinil (median dose of 80 ng/kg/min), two with subcutaneous treprostinil (median dose of 76.5 ng/kg/min) and five with intravenous epoprostenol (median dose of 28 ng/kg/min). They had been on these regimens for an average of 94.5 months (approximately eight years) before transitioning to Tyvaso treatment.
Before switching, patients received an oral combination therapy of a phosphodiesterase-5 (PDE-5) inhibitor in combination with an endothelin receptor antagonist (ERA). The transition process took approximately 56 days, and was conducted in the patients’ homes.
While the rate of subcutaneous injections or intravenous infusions decreased by 10–15 ng/kg/min every one to two weeks, Tyvaso was gradually increased up to 12 breaths, four times per day. Most patients (14 out of 16) ended up receiving a triple combo with Tyvaso in combination with a PDE-5 inhibitor and ERA. Patients were followed for a median of two years after transitioning.
Results showed that the transition to Tyvaso was generally well tolerated, and was not associated with significant alterations in WHO functional class, exercise capacity (measured by the six-minute walk distance test), or NT-proBNP levels (a prognostic biomarker of PAH).
In contrast, right heart catheterization showed significant improvements in mean pulmonary artery pressure (from 36 mmHg to 28.5 mmHg), and pulmonary vascular resistance (from 5.2 Wood units to 3.2) during the process of transition. Pulmonary vascular resistance is a measure of heart strain induced by high blood pressure in the lungs.
Patients receiving the triple combo reported less severe side effects. The most commonly reported side effects after transition included cough and headaches. Only two patients had to be hospitalized due to PAH, six months and three years after transitioning.
Overall, “for select clinically stable patients … transition to a combination therapy including inhaled treprostinil in the home setting appears safe, effective, and well tolerated, and offers an alternative to either continuous prostanoid infusion or to the inpatient transitioning protocols,” the researchers wrote.
“Transitioning at home is likely more cost-effective and may be more appealing to patients,” they said, noting that “patient selection, close monitoring, and follow-up remain essential for a successful transition.”



