Ion Transporter May Contribute to PAH Vascular Remodeling in Animal Study
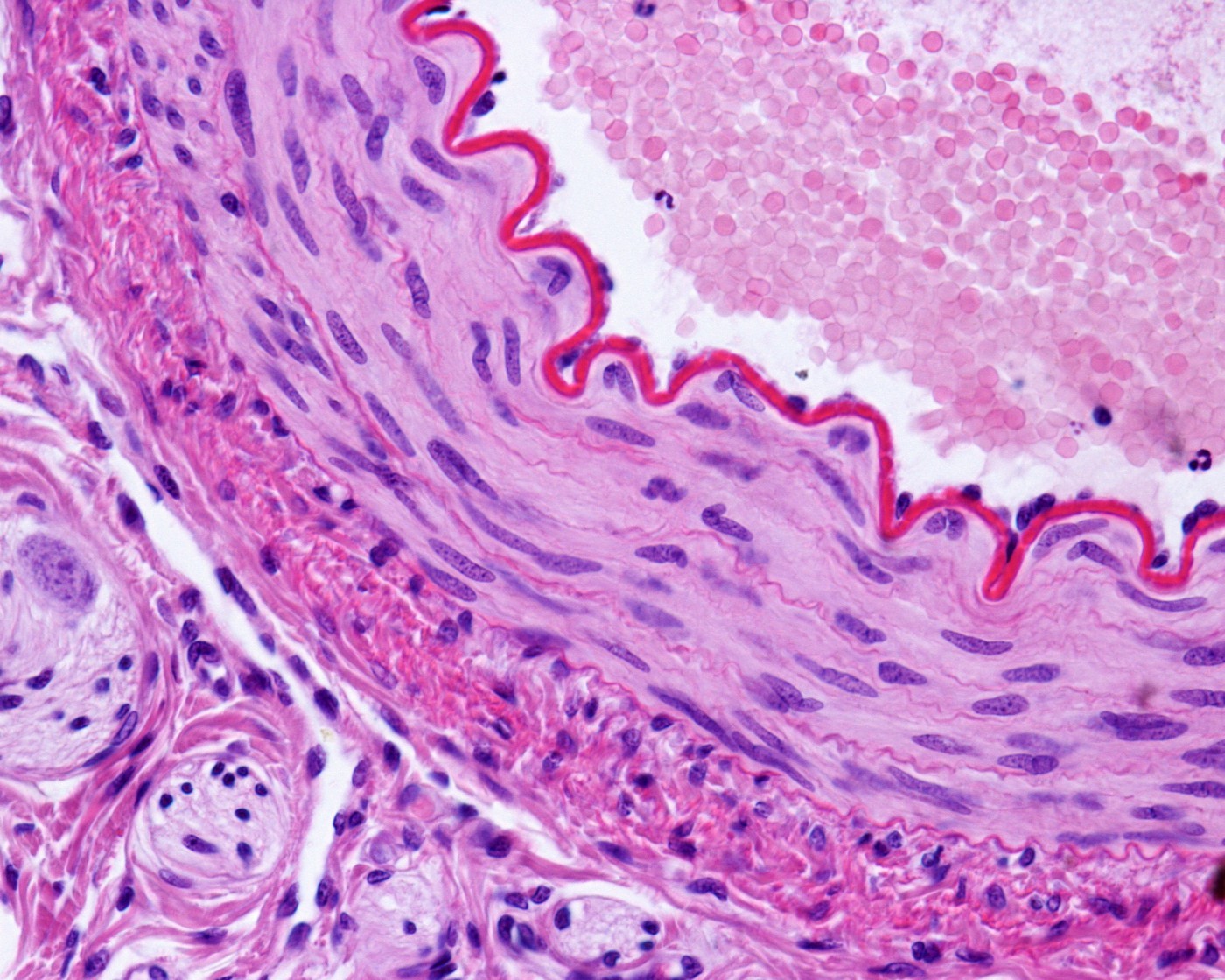
A study from Johns Hopkins School of Medicine showed that a cellular ion transporter might contribute to the increased expansion and migration of smooth muscle cells lining lung arteries in a model of pulmonary arterial hypertension (PAH). The findings provide new insights into disease mechanisms leading to blood vessel remodeling in PAH.
PAH is characterized by remodeling of the blood vessels supplying the lungs, but caused by factors still poorly understood. A mechanism that has been suggested to regulate the activities of smooth muscle cells in lung arteries is cellular pH, governed by ion transporters in the cell membranes.
One such ion transporter, the Na+/H+ exchanger, exchanging sodium for hydrogen ions, might be particularly important in regulating the functions of these cells. Previous studies have shown that it is involved in disease processes leading to pulmonary hypertension after hypoxia. Its role in PAH has, however, eluded researchers.
The study, “The Na+/H+ exchanger contributes to increased smooth muscle proliferation and migration in a rat model of pulmonary arterial hypertension,“ explored the ion transporter in a PAH rat model with extensive vessel remodeling. Researchers found that while the activity of the transporter was increased, the pH in pulmonary arterial smooth muscle cells was unchanged.
Studying muscle cells isolated from PAH rats, the team noted the cells multiplied and migrated more than those from control rats. When researchers blocked the ion transporter, the activity of the cells returned to normal levels. Interestingly, the transporter exhibited this increased activity despite its own levels being decreased.
Findings indicate that the ion transporter impacts the activity of pulmonary arterial smooth muscle cells in a manner that is not dependent on pH. The team could also conclude that the effects were not mediated by a signaling factor called ROCK, which can relieve the pulmonary arterial pressure in this PAH model.
The study, published in the journal Physiological Reports, also suggested that the activity of the ion transporter might be involved in a common pathway leading to blood vessel remodeling in various types of pulmonary hypertension.
Further studies are required to elucidate the exact mechanism through which the inhibition of the ion transporter alters the function of pulmonary arterial smooth muscle cells, and how the inhibition of the transporter could be used to prevent and/or reverse blood vessel remodeling.







