Now it’s Visible: Welcome to ‘Recharged and Rewired’
Anyone with a chronic illness is well aware that most conditions are invisible. What this means is that although our bodies tell us something different, we may look completely fine to the outside world. According to the Invisible Disabilities Association, an invisible disability is one that is “not always obvious to the onlooker, but can sometimes or always limit daily activities, range from mild challenges to severe limitations and vary from person to person.”
Congenital Heart Disease (CHD) has been my most challenging chronic illness, both physically and mentally, for the past 26 years. To the outside world I was a vibrant young woman who was full of life. I had good color in my face, wore a tan well in the summer, did sports and daily activities, just like an “average person.” I knew of my CHD, and was aware that I had a “special heart.” It didn’t bother me until around the time puberty hit, when my body began growing and changing. What was invisible to the outside world soon became extremely obvious to me.
Fatigue, shortness of breath, a dark purple/red face after skating an hour in a hockey game or practice, dizziness, black-out episodes, and chest pain started to be a huge part of my daily life around the age of 13. The hardest part about it was that people couldn’t physically see most of my debilitating symptoms. Aside from the bright red face, they didn’t notice the fatigue, exhaustion, breathlessness, black-out spells and dizziness. They didn’t notice because I never said anything. I denied what my body was trying to tell me. I denied it because I was afraid. Afraid of feeling different, and afraid of knowing there was something off in my body. I feared more surgeries, of not keeping up like everyone else, and was scared of the fact that I continued to push through it as if nothing was wrong. Fear in the chronic illness community is a very powerful feeling.
I spent my high school years, and most of my college years, denying what was going on with my body because I was afraid. It became visible when I began losing consciousness from overexerting myself, when the exhaustion left me in bed most of the day, when my coloring started going from a fleshy pink to a pale white, when my lips turned a whitish blue, and my body felt like ice. It turned visible when I had more scars across my body from a pacemaker implant and a cardiothoracic bypass surgery. The open-heart surgery scar was beginning to fade, but I had two new scars reminding me that I was not your average 23-year-old.
After my surgery, I started getting some color back in my face, returned to my daily routines, and began a career as a special educator. The problem with starting to look better is that people assume you are better. Around this time last year I was put on oxygen therapy for exertion. After having black-out spells more often, I took action and went to the hospital. I am glad I started to trust myself, knowing that something was not right.
After running stress tests and having me walk around the hospital floor, they noticed that with exertion my oxygen levels were dropping to the high 70s. I was diagnosed with chronic hypoxia, as a result of my vascular conditions and cardiac defects. This hypoxia over the years caused me to have pulmonary hypertension, which is currently being managed with oxygen therapy.
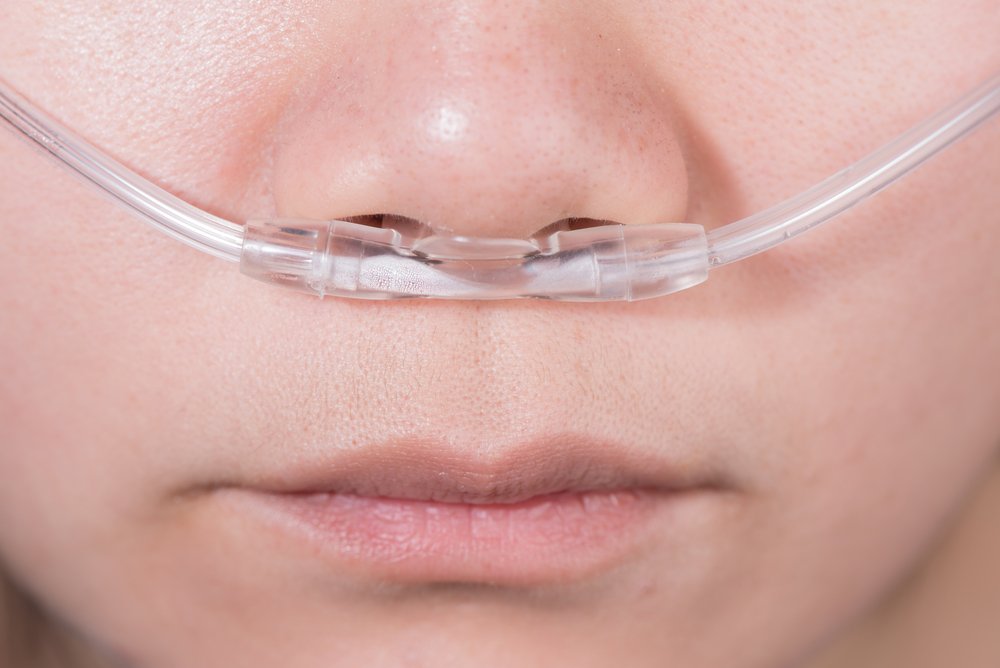
What was once invisible has become extremely visible. When people look at me, they don’t notice the scars, the pale face (thanks to the great color from that O2 flow), the blue lips, or the fatigued look. They now notice a nasal cannula, and wonder why an otherwise healthy-looking young woman has it. At first, I hated the fact that it has become more visible. Now I take pride in knowing that my visible disability is spreading some much-needed awareness for pulmonary hypertension and CHD.
I am not ashamed of my visible illness.
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.









Dave
Well said I'm 61 and was just diagnosed with PH in Feb 2017 and your very right people I know say wow your looking good. I'm now on oxygen and the same people say what's wrong. Even though you have told them before what you had. I was too embarrassed about wearing the oxygen but not anymore. Thanks again, Dave
Brittany Foster
Hi Dave,
It certainly is. I wear mine mostly with exertion so sometimes people won't see me wear it all the time and will say "so glad you are doing better." I feel like saying "same diagnosis, just a different day!" Glad you took the time to read the post and hope you enioy more to come!
Kathy LeCompte
Thank God for you Brittany and all of us who are afflicted with these
"invisible" illnesses. Unlike your defect, my defect went unnoticed my whole life until I suffered a bout of acute heart failure while on my job as a postal letter carrier. Being born in 1953, my defect went unnoticed even though I had failure to thrive, and was given a waiver to be excused from phys ed in high school, because I could no longer keep up with the other students as a result of breathlessness and excessive heart rates with any little exertion. Through all this no one ever noticed that it could be a serious problem. Now at 63 years of age, I'm barely hanging on, and have long since passed the golden opportunity to have my defect surgically corrected. To do so would probably cause me to have irreversible atrial fibrillation. It's high time people, including school nurses, and medical personnel noticed little people who look pale and grossly underweight, because to do otherwise sends a strong message to that child that nobody cares.
Brittany Foster
I agree with you so much that more should be done for the kiddos that keep pushing through it unnoticed. I feel as though it's a huge reason why there are so many cases of cardiac related deaths and drop attacks in athletes. Luckily I stopped sports around the age of 17 when I began getting a lot worse because I just couldn't take it anymore. Until I received the correct diagnosis, mine went diagnosed as "exercise asthma " for quite some time. Wonder why the inhaler never helped.... hmmmmm!!! Glad to be spreading some much needed awareness and hoping that it will get others the medical attention they need. Our bodies matter . Xoxo!!!