Finding PH Community in Waiting Rooms
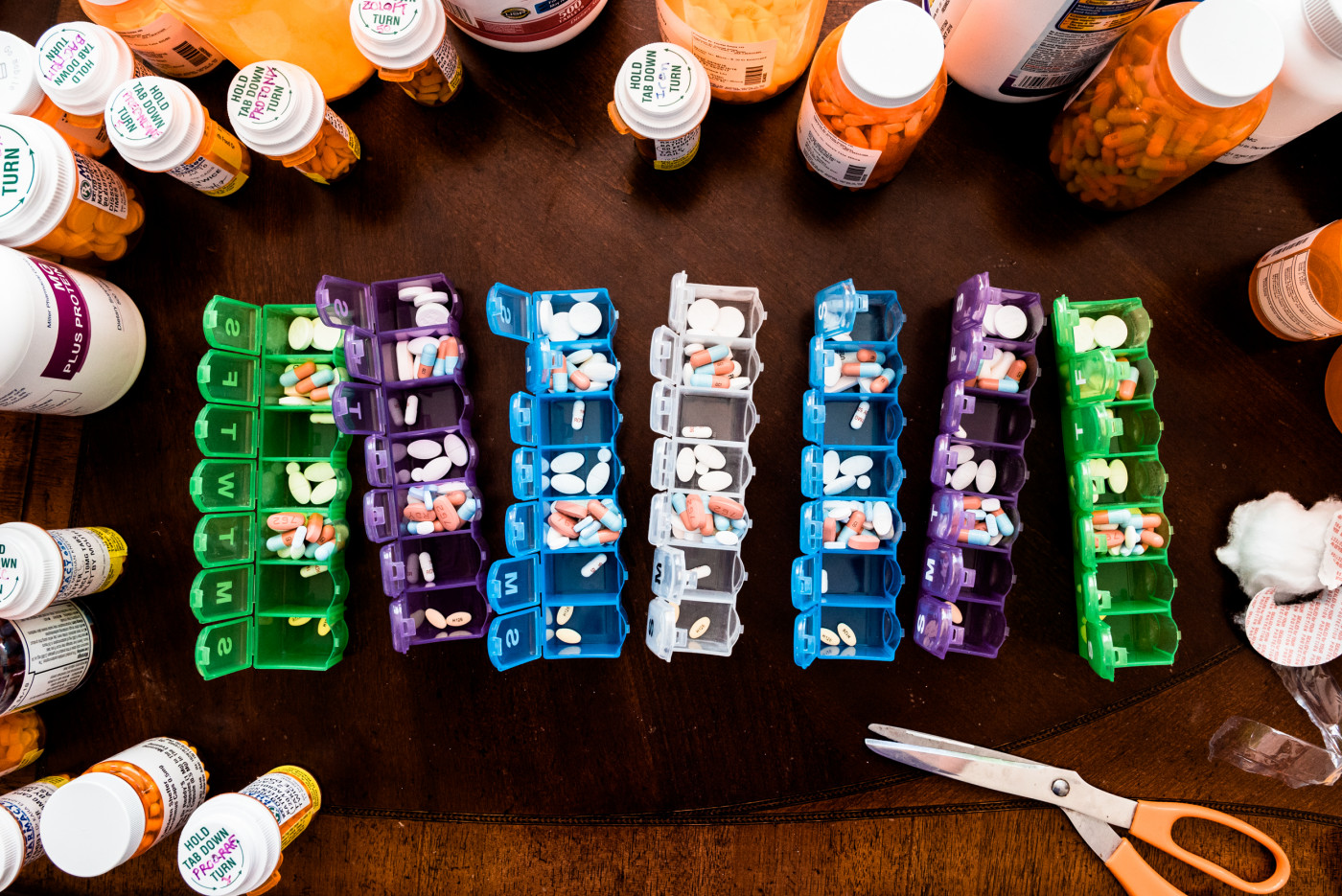
One week of transplant medications. (Photo by Kathleen Sheffer)
When my alarm goes off at 9 a.m. in the clinic and I pull out my bright green pill organizer, others around me start to do the same. “I’m glad she did that because it reminded me,” I hear one woman say as I leave the room to find a space where I feel safer taking off my mask for the five seconds I will breathe unfiltered air and sip water.
Lung transplant clinic days begin when I take a seat in a line of patients waiting for the pulmonary function lab to open at 7:30 a.m. Next, we race to complete chest X-rays and blood work before we can get our name on the list to see a physician. Some days I spend five hours at the hospital leading up to a five-minute meeting with my doctor. This isn’t unique to transplant clinics. Hospice physician Ira Byock recalls his father saying 20 minutes into a wait at a cancer center, “They give you only six months to live, and then, little by little, they take it back from you.”
Masks make it easy to recognize my compatriots, so I try to use time in waiting rooms to meet other transplant recipients. I carry business cards with a link to my blog to make it easier to stay in touch. I’ve met patients 10, 15, and even 20 years post-transplant, and heard stories about overcoming rejection and traveling internationally. Sometimes, it’s just nice not to be the only person in the room taking prednisolone, a drug that makes me pretty much constantly on edge and that has lived up to my pharmacist’s initial advertisement — more side effects than letters in its name.
The drug that kept me alive before my transplant was so uncommon that I had to fly or drive long distances to find other patients (and doctors) who understood it. My mom and I attended a pulmonary hypertension (PH) conference in 2000, a week after my diagnosis. A fire alarm went off in our hotel the first morning. Standing outside in our pajamas, we met other families attending the conference who, unlike us, had thought to grab backup supplies for their pumps that, like mine, administered intravenous Flolan (epoprostenol), a medication with a worrisome six-minute half-life. Forever after, I had a dedicated “backup bag” that went everywhere I did.
Biennial PH conferences were one of few forums in which I met other patients and learned critical information, like how to conceal my pump under a dress. Now I have a built-in community I can recognize based on the time they have their labs drawn.
Barring a few exceptions, all transplant recipients take an immunosuppressant with the brand name Prograf (also known as tacrolimus and formerly FK506) every 12 hours. Transplant teams have a target level for the tacrolimus concentration in the blood based on the type of organ transplant, time since transplant, and so on. You don’t want the level to be too low or you might reject your transplanted organ(s), but you don’t want it so high that you risk infection and toxicity. Because the level can fluctuate a lot while trying to find the right dose with a handful (literally) of other drugs, labs must be drawn frequently: 12 hours after the last dose and immediately before the next. For me, that means at 9 a.m. or 9 p.m.
Sometimes I’m just not in the mood to deal with needles in my veins right after breakfast. Luckily, a friend I met in a waiting room taught me the secret of the after-hours lab. When a father and son line up with me at 8:30 p.m., I’m certain they’re checking Prograf, so I introduce myself and ask what the boy had transplanted. Forever a perfectionist, I have them check in ahead of me so I can wait to have my labs drawn a little closer to 9 p.m. Out in the hallway, I overhear the phlebotomist praising the boy’s bravery. I smile, transported to bittersweet childhood memories.
As a child with PH, phlebotomists told jokes in vain attempts to distract me from the needle piercing my skin; my parents had me squeeze their hands, and they rewarded me with bags of chips after my blood was drawn. As an adult with a heart-lung transplant, I calmly pull down the arm rest, squeeze my fist, and take a deep breath. In a few moments, hundreds of thousands of other transplant recipients will be silencing alarms and swallowing pills. I am not alone.
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.












Leave a comment
Fill in the required fields to post. Your email address will not be published.