The Call that Changed My Life

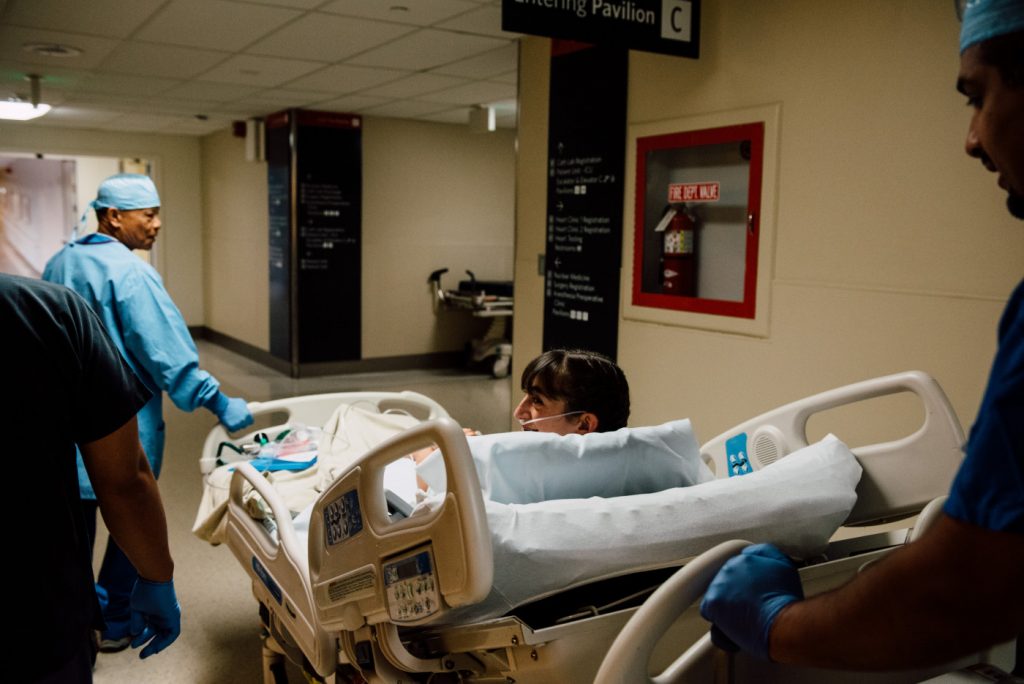
Getting wheeled to the OR. Photo by Monica Sheffer.
 As soon as the first words were out of his mouth, I knew the man on the phone was calling to offer me organs. I had imagined this phone call several times a day for the past month. He rushed through the script, stumbling over some parts. I eagerly confirmed I did not have cold symptoms and had not eaten since the night before. He promised to have a bed ready for me at 10 a.m.
As soon as the first words were out of his mouth, I knew the man on the phone was calling to offer me organs. I had imagined this phone call several times a day for the past month. He rushed through the script, stumbling over some parts. I eagerly confirmed I did not have cold symptoms and had not eaten since the night before. He promised to have a bed ready for me at 10 a.m.
The house filled with hurried footsteps and phone conversations. Excitement, fear, and confusion reigned. I didn’t stress about packing absolutely everything I needed because I believed it would be a dry run. Calls about transplants are never actually rehearsals, but they’re referred to as dry runs when, for whatever reason, the surgeons determine the organs are not viable. Most transplant patients I knew had gone through at least one — one friend even entered the operating room (OR) before the surgeon called it off. I figured it was a rite of passage; I would go through the motions today, but I still had a long time to wait.
Breathless and jittery, my parents, younger sister and I loaded into the car, each convinced we’d forgotten the most important item on the packing list we never finished making. It felt as if traffic moved slower than ever, specifically to heighten my unresolved panic. My heart had been pounding since the phone rang. Normally, my heart rate hung between 60-80 beats per minute (BPM), but on July 30, it was consistently over 100 BPM. However hard I worked to stay calm, adrenaline pulsed through me. Somehow, my heart knew this was our last hurrah together and was giving me every bit of strength it had left.
Friends arrived throughout the day, making this a festive occasion. We played card games, listened to music, drew henna tattoos on each other and laughed a lot. The anticipation electrified us all. Amid all the excitement, my donor was constantly on my mind. Knowing my donor and the family chose selflessness in intense suffering, my family felt at once connected to their grief and altogether separate from it. To this day, we celebrate my miraculous chance at life in the shadow of the loss that made it possible.
Aware of the risks that came with this chance at life, I solicited my friends to witness an advance directive and forwarded my mom the informal list of final wishes I typed in a note on my phone during a bleak period in college:Iinstructions for how long to keep my Facebook profile active and various demands for the party I want in lieu of a funeral. Waiting outside the doors to the OR with just my parents, I apologized for some of the more outdated requests. In the two years since I started planning for end-of-life, my prized possessions have changed and friendships have evolved, along with my social media passwords. During what could have been our final moments together, my mom and I spoke animatedly about where to direct donations in the event of my death. Over-preparation was one of our practiced coping mechanisms.
While surgeons transported and visualized the donor organs, I lay in bed, watching nurses carefully arrange clanky instruments, their backs turned to me. Behind me, my gentle anesthesiologist tended to his assigned tasks, intermittently making small talk. He had me choose a Pandora station. That this might be the last playlist I listened to, as an accompaniment to my operation, added a whole new level of pressure to a decision I normally leave to more musically literate friends. After intense deliberation I settled on Blind Pilot, and felt relieved that the only complaints pertained to my anesthesiologist’s lack of a paid subscription (we listened to ads between songs).
Hours later, someone announced the donor organs looked great, and the team was ready to begin. “Uh-oh,” I thought. “This is not a dry run.” With the infusion starting to put me asleep, I felt lucky to be the patient and have nothing left to do but trust my body and my team. The real work would begin when I awoke.
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.









Leave a comment
Fill in the required fields to post. Your email address will not be published.