Camille Frede Receives a Long-awaited Heart-lung Transplant

Kathleen and Camille in 2014. (Courtesy of Kathleen Sheffer)
On Sunday, one of my longest friends with pulmonary hypertension received a heart-lung transplant. I met Camille at the first PH Conference I attended in 2000. I was 6 and she was 10, so it was a big deal that she even talked to me, let alone befriended me. Ever warm and enthusiastic, Camille took me under her wing and introduced me to new friends and ideas about life with PH. Her mom supported my mom by email for the first few years after my diagnosis, and our families spent time together every other year at Conference. The last time I saw her in person, back in 2014, she had gotten fit and muscular (especially by PH standards), and showed me some exercises I could do safely (I didn’t stick with them).
Camille began the transplant evaluation process around the time that I had my surgery in 2016. Our roles reversed; I’d always looked up to her, but now she had questions for me. A nursing degree under her belt, many of her questions went over my head. It took me months to want to talk to anyone with PH about my transplant. I struggled to be an example of strength when I wasn’t feeling emotionally stable. Adjusting to all the changes of post-transplant life, I felt like I’d acquired a much more demanding illness, and I hadn’t yet seen all the ways it would enrich my life. Luckily, I recognized that at the time and tried to abridge my list of woes.
Camille went on the heart-lung transplant list at Brigham and Women’s Hospital in Boston on Oct. 19, 2017. Hospitalized since Feb. 5, 2018, the team told Camille she might have to wait a year for transplant. She told me she wasn’t sure she could wait that long (I wasn’t sure, either). She went forward with dual-listing at another center in the area, and considered traveling all the way to California to list at Stanford, where doctors predicted a shorter wait time.
On March 2, just under a month into her hospitalization, doctors started her on veno-venous extracorporeal membrane oxygenation (ECMO). The technology, largely derived from cardiopulmonary bypass, performs gas exchange outside the body. Cannulae placed in the jugular vein removes blood from her system for carbon dioxide removal and oxygenation of the red blood cells. Hearing that Camille would start on ECMO worried my dad, a registered nurse, because it comes with many potential complications. Honestly, I’m glad I didn’t even know it was an option when I was transplanted because my hands shake just writing about it now.
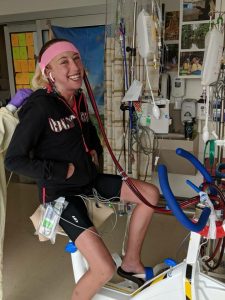
On Saturday, March 24, Camille rode 15 miles on a stationary bike in her hospital room while friends hosted a fundraiser and 15-mile bike ride of their own back in Michigan. Yes, that’s right, she rode 15 miles while essentially on heart-lung bypass. Camille has fierce determination!
After 48 days in the hospital, 22 of them spent on ECMO, Camille received a call offering her a donated bloc of heart and lungs. She went into surgery the morning of March 25. I’m so grateful to her donor and their family who made the selfless decision to give the gift of life. Though I’ve been waiting and hoping for this opportunity for Camille, I recognize it comes at a time of great loss for another community. Their decision to make some meaning out of a tragedy inspires me, as does that of my own organ donor.
I’m writing this as Camille comes out of surgery. Her new heart looks great, but her donated lungs have too much fluid in them. The surgeon needs to keep her intubated on ECMO with her chest open for a few more days. This is not an uncommon situation, I’m finding, as I meet more and more transplant recipients. Camille has a long road to recovery ahead, but her tenacity, reinforced with over 24 years battling pulmonary hypertension, will surely carry her through. As for me, I have some training to do so I will be able to keep up with her on bike rides!
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.










Kaye Norlin
Awesome! Prayers and good thoughts for her!
Kaye Norlin
PS I was on ECMO with no problem. So here's hoping.
Steve Van Wormer
http://phawarepodcast.libsyn.com/episode-142-camille-frede-rn
Camille Frede, RN is from Grand Rapids Michigan. She was diagnosed with pulmonary hypertension at the age of four. Camille became a nurse because she wanted to give back to her community and advocate for her patients. She uses the gift of being a patient herself to mirror her empathy for others. This interview was conducted while Camille was in the hospital awaiting a heart/lung transplant. After 48 days in the hospital and 23 on ECMO, she received the call on 3/25/18.