With a Lung Disease, ‘Breathing In and Out’ Isn’t as Simple as It Sounds

“Focus on breathing in through the nose and out through the mouth.”
ER doctors told me this as I tried slowing my heart rate down after feeling palpitations following my numerous breathing treatments. My heart rate eventually went down with the help of medication and my breathing finally became more natural. This entire experience made me realize an eye-opening truth about my cardiac and pulmonary conditions. Now, not only is my heart rate controlled by a pacemaker and various medications to keep me from having an arrhythmia, but my breathing is also assisted with the help of medical equipment, oxygen, medications, and breathing treatments.
Before my pulmonary complications, I took breathing for granted. “Breathing in and out” is not as simple as it sounds for many with pulmonary hypertension. Breathing should be a process that people don’t give much thought to throughout the day. It should be an instinctual action. For me, it feels anything but instinctual most days. To be able to breathe somewhat comfortably, and exchange gases sufficiently, I have to rely mostly on modern medicine.
For many with pulmonary hypertension, relying on the rhythmic and involuntary pattern of our own breath is a thing of the past. Breathing takes effort and medical intervention compliance. Over the past few years, breathing has become more of a conscious effort. To properly breathe, I require oxygen usage, medications, inhalers, and breathing treatments, BiPAP, and numerous procedures and monitoring.
I’ll be the first to admit that I HATE wearing oxygen for numerous reasons, but stopping to study how exactly it helps me to breathe reassures me it’s good to wear it. Oxygen is essential because it goes through the entire circulatory system and helps to energize the many cells of the body. Breathing allows for the exchange of oxygen in the lungs and proper ventilation. Without enough breath, the body feels exhausted, the mind gets foggy, muscles become weaker, and bodily processes decline.
People with pulmonary hypertension take many medications throughout the day. For example, I have taken prednisone to help open up the chest to allow me to breathe better. It doesn’t come without side effects, but it is an effective medication, especially if there is any inflammation in the chest or lungs preventing someone from breathing properly or raising their oxygen levels. I also take antibiotics frequently for pulmonary infections that occur as a result of my inability to clear out my lungs properly due to a weakened cough. Recurring bronchitis and pneumonia can lead to extra complications for anyone with pulmonary disease.
The upper airways must open up to breathe. To ensure this, I rely on inhalers and multiple breathing treatments throughout the day. Chronically low oxygen levels constrict my airways. With very low oxygen, sometimes my throat muscles go into a spasm, making it harder to suck air through my throat — it almost feels as if I am choking. My breathing treatments and inhalers help to relieve this uncomfortable sensation and allow my upper airways to relax enough for me to focus back on breathing.
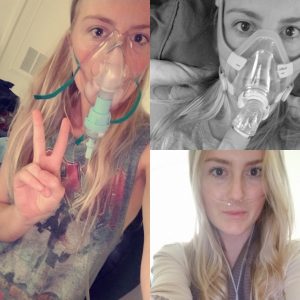
(Courtesy of Brittany Foster)
A BiPAP machine helps me with the actual act of inhaling and exhaling. Throughout the day, there are times when I struggle with the actual act of breathing in and out. The BiPAP machine allows me to take in a big enough breath and gives my chest muscles a break from having to do it on their own. It’s a break for my muscles and mind when I don’t have to give breathing much effort and thought.
All of these various interventions have slowly become second nature to me. The more I do these things, knowing what they’re helping me with, the more it feels like I have the control over how well I breathe each day. Breathing shouldn’t have to be something that I think about more often than not during the day, but it is. I do these interventions in hopes that one day I won’t need to be coached to “breathe in and breathe out.”
Has breathing felt less natural for you? Do you notice that breathing feels more like an action that takes effort? What medical interventions, medications, or equipment help you to breathe better during the day? Join the PH News Forums post about this topic.
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.









Leave a comment
Fill in the required fields to post. Your email address will not be published.