Medication Compliance and Patient Advocacy Are Big Pills to Swallow
Written by |
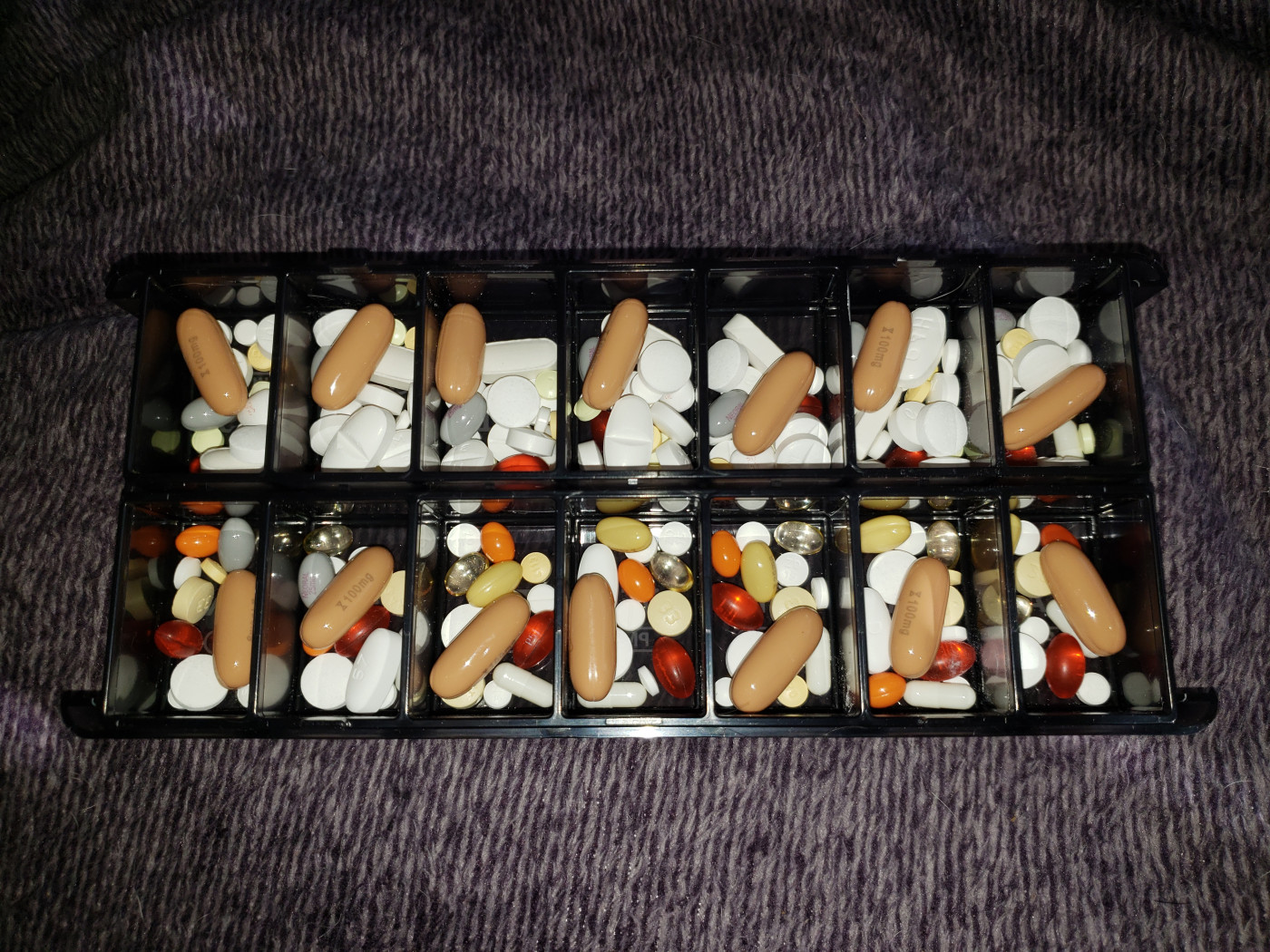
Cullen’s medications six years after transplant. (Courtesy of Colleen Steele)
Learning how to take medications can be a hard lesson for children, but my son Cullen managed it like a champ when he was diagnosed with pulmonary hypertension (PH).
I know adults who struggle to swallow pills, but at 8, my son could take them without issue or complaint. It was the oral treatments that came in a liquid form that he despised, even more than his continuous intravenous Flolan (epoprostenol GM) therapy.
Unfortunately, he had a few liquid medications he had to force down for several years until he outgrew the pediatric dosages. Having a treatment switched to a pill was as exciting for him as losing a tooth or getting training wheels off his bike.
I asked Cullen if he has advice for PH patients with a phobia of swallowing pills or drinking liquid dosages. “If they want to live and hopefully experience a better quality of life, then they need to get over it,” he said. I’m sure many will find that advice a hard pill to swallow, but it is the reality of the disease.
A willingness and an ability to take medications in any form and on time are a big compliance requirement when being considered for transplant eligibility. Cullen’s medications multiplied after his heart and double-lung transplant, and six years later, the number of daily pills he takes has barely dwindled.
To keep his new organs healthy and treat the coexisting conditions that developed after transplant, he takes an average of 30 pills a day, sometimes more when dosages change. Cullen explains that out of respect for his donor, he takes them without complaint. Instead, the regimen is a daily reminder to feel grateful for his second chance at life, and thankful for the pills that help protect the precious gifts he was given.
Cullen likes to take the worst-tasting, horse-pill-sized medications first, then swallow the rest all at once, in small fistfuls with a lot of water. Whether you take your pills one at a time or all together is up to you, but Cullen stresses that you should ask your doctor about following a specific order when taking certain drugs.
Also, ask if you should take medications with or without food. A small snack usually helps Cullen stave off nausea, but eating too much before taking his medicine often makes him feel worse. Find a balance that works best for you.
As a PH patient, you should know your medications. But if you are a transplant recipient, it is required that you know them well. This includes the generic (or chemical name) and brand name of every treatment being taken, the dosages, what they are for, and the side effects they can trigger.
In addition to knowing your current medications, experience has taught us that it is just as important to keep track of what you have taken in the past. We maintain a list of former medications that Cullen has taken and keep it in a medical binder he takes to appointments, emergency room visits, and hospital admissions. We include the date of when he started and stopped treatments and why they were discontinued. This is an effective way of helping Cullen advocate for himself, and doctors often appreciate a patient who knows their medical history.
Over the years, Cullen has learned the hard way that he is allergic to several medications and many supplies used to maintain the various types of intravenous lines he has had as a PH patient and a transplant recipient. It should go without saying how important it is that you know your allergies and the symptoms exhibited with them. But another lesson experience has taught us is that it’s very helpful to know what you can take in place of what you are allergic to.
For example, Cullen is very allergic to several anti-nausea medications. Many times, exasperated nurses will ask, “Well what can you take?” It’s helpful to them, but most importantly, beneficial to you if you are able to answer that question.
It is strict hospital policy that medications can only be taken if given by staff. They would rather you not have your home medications on your person when admitted. But when Cullen was a PH patient, he had skin allergies to the most commonly used central line and PICC line dressings. Hospital staff welcomed what we brought from home that could safely be applied. We always kept our ready-to-go hospital bag well stocked with them.
Help your medical team help you. Take your medications on time. Know what they are and what they are for. Know your allergies and what you can take in place of them. Be your best self-advocate.
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to pulmonary hypertension.




Leave a comment
Fill in the required fields to post. Your email address will not be published.