Pulmonary Hypertension News Forums › Forums › PH Care and Treatment › Exercising With PH › Mowing the lawn and O2 sats
-
Mowing the lawn and O2 sats
Posted by brenda-denzler on April 13, 2022 at 5:24 pmQuestion for everyone:
I mowed today for @ 30 minutes. Self-propelled mower. Thought I was going to cough a lung out, with the grass and pollen and dust thrown up. Had to put on a mask to protect my airway.
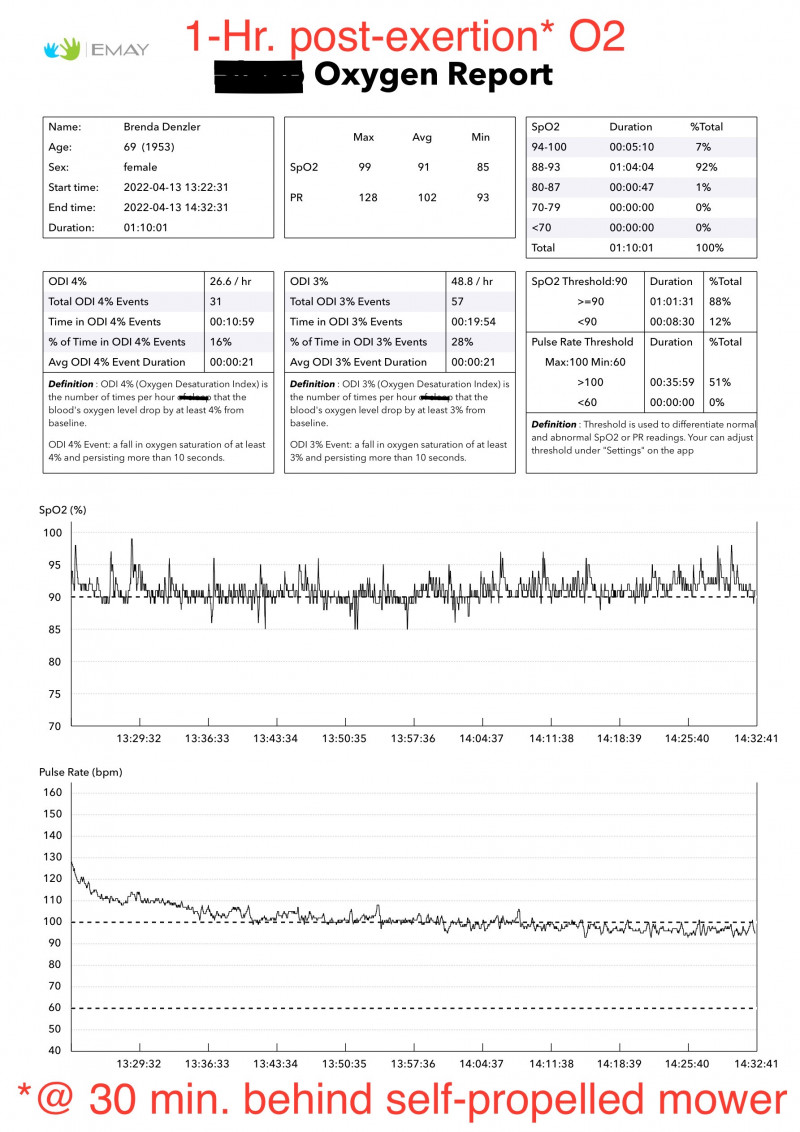
Staggered into the house at the 30 minute mark and sat down with a pulse oximeter that takes continuous recordings. I sat with it on for just over an hour while I tried to recover so that I could get up out of my chair without feeling like I was about to collapse. The accompanying picture is the result.
Note the amount of time in the hour AFTER I had exerted myself when my O2 reading was below 90%. And note the number of times my 3% and 4% oxygen desaturation index occurred. And this was while I was awake–I wasn’t sleeping. I was just sitting quietly.
Can anyone here say, “Yeah. That readout looks like something I get (or used to get) when I’d exert myself, like doing work or exercising.” Or does this look like something a bit different in some way?
OK. I guess I can’t put the graphic in here. No matter how I try, I can’t get the program here to accept a JPEG. <<sigh>> Any ideas how I can share my data with you folks?
jen-cueva replied 3 years, 2 months ago 3 Members · 16 Replies -
16 Replies
-
Hi @brendad53, I am concerned about you mowing the lawn, self-propelled or not until you learn more from the test and Dr. Ford. That dust and air only increased your breathing difficulties, not to mention the elevated heart rate and decreased oxygen saturation.
I’m no doctor, but this is concerning to me, and I hope you can find someone who may do this task for you. Unless you ask Dr. Ford and he agrees this is not an issue, I would take not try and tackle this chore. At least not until you can start on treatments after getting some more answers, my friend.
Regarding posting this image, members don’t have that option, unfortunately. I did agree to accept this one because I knew it was related to your post above. But anytime, you can send Colleen or me an image, and it’s possible that we can post it for you. I’m sorry if this causes any inconvenience. It’s forum guidelines.
How are you feeling today after this grass-cutting marathon?
-
Jen, the test won’t be until early September. That means an entire growing season of me needing someone else to mow my grass (such as it is!). I’ll see what I can manage, but am not confident I’ll be able to do anything. Except wear a mask when I mow. It really did irritate my airways when I was mowing without the mask. The good news is that my older son and his SO gave me a battery-powered weed whacker that they no longer use. It’s lighter weight that my gas whacker, so it’s easier to use. That’s nice.
Today I’m feeling very exhausted. Moving very slowly. Can’t begin to think of doing yard work today. Too exhausted. Went to cancer hospital to talk to my shrink this morning, and it was all I could do to walk between the parking deck and the hospital—but I figure it’s good exercise, right? Today I’m going to have to take it kinda easy. It’ll take me 2-3 days to recover from yesterday.
That’s what most people don’t get. They see me go to a grandson’s little league ballgame or hear me say I mowed the north yard and back yard, and think I’m doing alright. What I don’t say is, “It will take me a couple of days to recover from this exertion. I barely had enough strength to take a shower, later in the evening, but I was so sweaty and dirty and gross that I pushed myself to clean up. That used up energy I didn’t really have to spare.”
I am touched that you are concerned, Jen. It seems that few people in my life are, so I am touched when someone “mother hen’s” me. I’ve shared the above test results with Dr. Ford and copied my PCP. I also shared them with my shrink this morning. He said, “This is real data, Brenda!” And I said yes. Then he said that if I were in the hospital with those readings, I probably would have been given oxygen. I agreed that this thought had occurred to me, too. We’ll see if Ford or my PCP respond in any way.
But…*are* these the kind of readings that people with PH might have, in such a situation? Does this look familiar? Or does this look like “Something’s going on, but it doesn’t look much like the pattern I know from PH”?
-
I wish you had another option for the lawn. Like Jen, I don’t think you should be doing it. Could you hire a teenager? My son is 12 and would love to do that kind of work. I know how you feel about having this invisible disability. You look fine, so it’s hard for people to understand that you really are not fine at all. I was almost relieved when I had to go on oxygen, partly because it allowed me to do more things but also because it was like proof there was really something wrong with me. I can imagine it’s even tougher for a guy because you’re supposed to be strong and do all those tough outdoor chores. I would maybe call the doctor and ask what they recommend. If they tell you not to mow, you have doctor’s permission/requirement to find another option. By the way, how did you get that oxygen report? What kind of oximeter do you have?
-
Hey, Cathy. I can’t hire anyone to do this. No $$$. I may be able to get my two grown boys to come help, but experience has shown that this, too, is very difficult to manage. They have lives and families of their own, and they’re very busy.
Can you give me any idea about WHY I shouldn’t do this? I mean, what could happen to me, if I persist in mowing my lawn and I am having oxygen problems like this? Anaphylaxis? Heart attack? Collapse to the ground and unable to get up? What *could* happen, if I persist in doing my own mowing?
I’ve had the same thought about going on oxygen. It would be “proof” that something is really not right. One of the greatest blessings of my recent life was when two friends from out of state were visiting and we went to the mountains, where I had a bad, bad, bad spell. Scared them to death. They thought I was having a heart attack. Told me later that I was very, very pale. I could barely muster the energy to move. I had every piece of clothing I owned, plus four layers of bedding on top of me, but I was chilled to the bone and couldn’t get warm.
This happens on a distressingly regular basis. But I live alone. I try to tell the doctor, but it’s just me saying things, y’know? There is no context for telling most other people about what happens, and they understand it even less than the doctor. But when I went to the doctor and said my friends had made me swear to consult with him (again) about this, and I could give concrete examples of things I couldn’t do because I was so symptomatic…. That made a difference.
I’m about at the point of asking for a handicapped placard. Sometimes it’s a pointless use of scant energy to park further away from anyplace and walk in. My friends who visited and saw me have a bad episode? One of them has a handicapped placard, which we were using for her. I was never so glad as I was then. I needed it almost more than she did!
Oximeter I use is an Emay Bluetooth Oximeter. It records a reading every second (if memory serves) and averages out each 60 seconds-worth of readings to display a 1-minute reading. So if you wear the oximeter for an hour+, like I did the other day after mowing, you get a moving picture of your heart rate and your O2 sats. The data is uploaded to an app (which I have on my phone), and turned into a graphic you can view using the app. You also have the option of downloading the data as a CSV file (for importing into something like Excel) or as a “report.” What I posted, above, is the report. You can save it as a PDF or a JPEG. I find it easier to annotate JPEGs, so I’m starting to switch to that format for my reports. If you PM me, I’ll try to find the oximeter on Amazon and post a link to it. (Not sure that would be permitted in the general group, here…?)
-
-
-
Hi @brendad53, Yes, sadly, others have no clue when they see or hear about things we can do. The recovery period or downtime for me depends on how I am before the activity and other data that affects how fast or slow I bounce back.
I’m hopeful this reports some insight for the doctors; maybe they can order oxygen based on this data. That is a ton of information. I’m sure that you may here find this helpful. If I have the correct item on Amazon, the price point is excellent for that much data.
You ask if others see these readings and complications, I can attest to that and say yes to some extent when I was first diagnosed. I haven’t continuously monitored my oxygen sats with activities but would hope it has improved.
Yes, you can pass out or have syncope, which many do, go into heart failure and other complications. But without knowing much about your diagnosis, level where you are, etc., it’s hard to say. It’s certainly concerning, and I hope you can find a family friend or your sons possibly rotate to help for a bit. Please be careful.
Do you have any organizations in your area that volunteers to do things like this for others who can’t? Most communities do, once we learn to accept help. I’ve been there stubborn and didn’t want to give up any of my chores.
Yes, feel free to add links; those are approved by myself or Colleen. This protects hackers from sharing links on our sites.
Is this your pulse oximeter on Amazon?
-
Yes. That’s the one I have. And I agree. It’s a lot of info for a reasonable price. Exceptionally reasonable today with that flash sale! And as my product evaluation on the site says, I was very impressed with the responsiveness of their tech support folks, when I couldn’t make mine work. They weren’t just giving me the brush-off, quick response to my concerns. They spent time and worked with me.
I’ve been monitoring my sleep O2 levels ever since I got this particular oximeter, and recently my sleep sats have gotten low enough consistently enough that I have admitted I now need a proper sleep study. So that’s in progress.
I will call the senior center and see if someone can help me with mowing this summer at a free/very cheap rate, explaining that I’m in a long process of trying to get a diagnosis for this.
I’ve also contacted my PCP and asked him if I would have better functionality if I had O2 to use when I mow…though how I’m going to have an oxygen canola in my nose and yet a simple pollen/virus mask over my nose at the same time, I can’t quite figure out! I would have asked Ford about this, but I don’t know him well and am kinda embarrassed to bring up such a thing with him.
The thought of passing out while mowing isn’t a big concern. The mower would stop when I let go of the handle. No danger. But heart failure is a bit more concerning. I’m not even sure what “heart failure” is (symptom-wise), but I know I don’t want it.
-
Hi @brendad53, thanks for sharing that helpful information about your pulse oximeter. It’s much appreciated by myself, and others will find it useful.
Hopefully, your doctor will want to order oxygen or at least an oxygen study, oximeter test, which you pretty much have for them already. I’m sorry that your stats are low, but happy to hear that you’re finally on board to have a sleep study done. Those who use a BIPAP and CPAP have noted some improvements after starting those.
Yes, please call the local senior center to see if they have someone who can volunteer. Many offer these types of things to help for free. Please keep us posted on how this goes, and the sooner, the better.
I also tagged you in another topic about heart failure and PH so you can read about others’ experiences. Take care and please try and take it easy.
-
Jen, thanks for the referral to the heart failure group. I’ll be reading up on that, shortly.
As for my results that I posted above: I asked my PCP if portable oxygen while I tried to mow would be possible. He forwarded the query (I’m guessing) to Dr. Ford, who looked at the data and said we should get a 6-minute walk test on me to see if I could qualify for portable oxygen.
I appreciate his effort to be responsive. However, I *will* pass a 6-minute walk test. And I told him that. Yes, I”ll do the test. But I know already how it will turn out.
As a way of showing how it will turn out, I put on my oximeter and tried to do my own “activity” test a little while ago. The device didn’t work 100% of the time. There are gaps in the data, where the oximeter and my finger failed to find each other so there was no recording. But I did get some solid data–albeit in chunks of time, not as one dataset. I’m having to piece it together using Excel, because the oximeter app won’t collate individual readings.
The bottom line, however, is that while I was active I never once desaturated. And in fact, my sats went UP.
And this is my dilemma. It’s not what you expect from someone with a heart condition or PH. Yet if I’ve been up and really been “working hard” like mowing, the **after exertion** results are like the Emay Oximeter report shows.
So my pattern is: (1) Resting O2 around 92-95; (2) Moderately active O2 around 94-97; (3) Post-exertion O2 after significant effort is upper 80s to very low 90s.
Makes no sense, does it? As I told Dr. Ford, there doesn’t seem to be an ICD code for this.
-
-
Hi @brendad53, I wanted to check in and saw how you’re doing this week. Did you have any luck getting oxygen from your doctor after your readouts?
-
Well, things have progressed slowly and on wobbly paths, as seems usual. Dr. Ford, the pulmonologist, has not responded to my comment that yes, I’d take a 6-minute walk test, but I was sure I’d pass it. The test has not been scheduled yet, so I don’t know if he’s re-thinking the need for it or re-thinking his understanding of the pattern of my O2 deficits. Or it has fallen between the cracks.
Meanwhile, my PCP, Dr. Barnes, was copied on the EMAY post-exertion report. About a day later I wrote to him to ask if he thought it might be *easier* for me to mow if I had portable oxygen. He wrote back to say that he thought it was entirely safe for me to be doing my own mowing, which of course did not address the issue I had raised. (Anxiety moment #1.) He went on to say that the O2 readings I had shared weren’t all that terrible, when you averaged out the numbers. (Anxiety moment #2.)
I responded to him, saying that the issue for me was not safety. It was ease. No response, and it’s been a couple of days.
Tuesday night I listened in (mostly) to the CTEPH phone support group. At the end the leader (I got there late so did not catch her name) asked everyone to say who their biggest supporter was, in dealing with this disease. Every single person named other people who stepped up and did things for them—physical things, like chores. Or who noticed when they were getting too tired and would tell them to go sit down and rest. It made me cry. I am having trouble getting the people around me — including my physicians — to act, consistently, like I do have a medical problem of some sort that needs to be dealt with. I’m at the stage of just trying to get acknowledgement that, “Yeah, you’re a bit sick.” I haven’t even gotten that far, yet. Then the next step is to have people in your physical space who can and will help you do things from time to time, when you can’t do them yourself. I have no one to rely on like that. Thank God for one neighbor, who has recently helped me do two big tasks that there was no way I could do alone. And a close friend who helped me with a landscaping project. And now a long-distance friend who is helping me get some assistance with the mowing—a recurring need that I’m going to be trying to handle this summer. Feeling a bit like Blanch DuBois. If it weren’t for the kindness of these strangers, where would I be?
I doubt, Jen, that I will be getting any O2 of any kind. When my shrink saw the EMAY post-exertion report, he commented that if I had been hospitalized at a time like that, he suspects I would have been given oxygen. My pulmonologist says we should probably do a 6-minute walk test to see if I can qualify for portable O2, but may have misunderstood what “POST-exertion” meant when he saw the EMAY report. My PCP thinks the numbers in the EMAY report are not terribly concerning, when you average out the highs and lows.
So today I sprayed some Round-Up (evil stuff) on a gravel drive, pulled weeds while sitting down for about 30 minutes, played fetch with my puppy for about 15-20 minutes, and am now needing a nap. When I wake up, I hope to do some data entry for about 1-2 hours, and that will be my accomplishments for the day.
I’d be interested in hearing your story, Jen. Starting with “these symptoms that nobody could figure out,” to the Level 3 CPET that helped them name it, to where you are today with symptoms, treatments, functional levels, etc.
-
Oh mo, @brendad53, this certainly must be frustrating in many ways. I hate to hear that you aren’t getting much support from loved ones, friends, or the medical team with your concerns.
I’m thankful that you could listen to the CTEPH support call but sad that it upset you to learn that most do have support at home. I must say, without my hubby, Manny; I don’t think I could do this. So, I applaud you, although I also worry when we have those like yourself living alone.
I wish I could tell you more about my testing, but it was so long ago and pre-COVOD that I can’t recall all the essential details. I know I couldn’t finish the test. But Dr. Channick, who was at UCSD and then Mass General, now UCLA, did my test. When some of the details start coming back, I’ll share them with you. But with my brain fog, it’s challenging to think about that long.
Brenda, I wish I had better words for you. Please know that you’re in my continued thoughts and prayers.
-
Thanks, Jen. I’ve been thinking about the “support at home” thing, too. And I’ve about decided that my situation is not altogether undeserved. I have done things in my life, I think, that have put me in the position I’m in now. So sympathy for me may not be entirely deserved.
As for the doctors…that’s always the way it is for me: The world of medicine is inadequately responsive, confusingly responsive, or downright unresponsive. On blessed occasion, it is responsive, correct, and timely. But those occasions are notable because they are not a consistent feature of what it is like for me to get health care.
-
Hi @brendad53, don’t be so hard on yourself. We all make mistakes and deserve love and understanding. Allow yourself a little grace.
Also, hold on to those few positive experiences with the medical community and hope that will change. I’m sorry that you feel so unheard, unvalidated, and confused.
Did you hear any more about the 6-minute walk test? Were you planning to have it done to evaluate your oxygen needs? Are you waiting to see what the testing in Boston reveals?
-
-
-
Well, Jen, I’m not sure it’s being hard on myself. I think it’s being honest with myself. I did a lot of things right, raising my boys. But I also did some key things poorly, as compared to how I wish I’d handled those things. To be honest, though, I did the best I could under the circumstances. I don’t think I could actually have done any better. Just the way I am, and the way things went down.
As for my doctors, I do hold onto those good moments. And with time and experience, I’m getting somewhat better at managing my interactions with doctors so that I’m less reactive. Which increases the chances that I’ll have better interactions. But like I noted, above, the smallest things can trip my “anxiety wire.” My PCP just did, about this whole EMAY report thing. And I love my PCP. He’s one of the good ones. But this time he triggered my anxiety, and I’m sure he never even knew it. A good deal of the credit for “good interactions” lies with the doctors themselves. Some doctors get it right. They are amazing.
I haven’t heard anything more about the 6-minute test. I’ll nudge the pulmonologist in a few days if I don’t hear anything more. But I will, of course, pass it. I plan to schedule it later in the day and then wear myself out before I show up for the test. That way, instead of getting my fresh, “best” effort, they’ll get my “I’ve been on my feet for a while” effort, which will be considerably less impressive.
-
Hi @brendad53, I love that you mention many things you should have done better in life. You are not alone. I have had many occasions where I could have done better. We are human.
With your doctor interactions, I’m proud of you for learning how to be less reactive. Although we know this, we also are our best advocates. From what you’ve shared, I think you do an excellent job advocating for yourself, Brenda!
Please let us know once you have the 6MW test scheduled and how we can best support you.
Hopefully, the weather is warming up, and you’ll enjoy more fresh air soon. Take care of yourself.
Log in to reply.