The Big Unveil: Gaining Closure After My Transplant
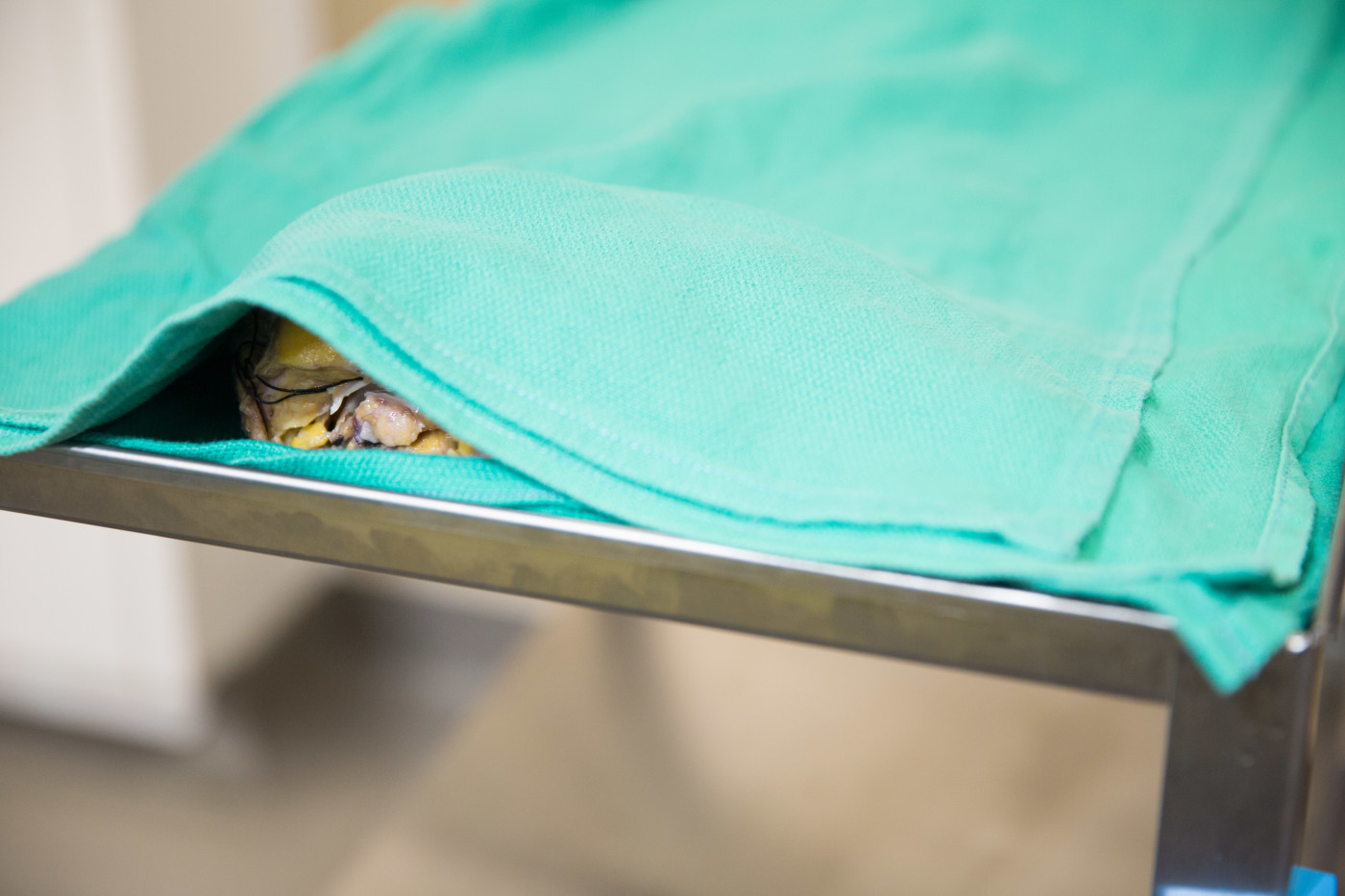
Photo by Nick Otto.
I was spending time with a friend, another long-term PH survivor, at a cafe last week, when she picked up a phone call. A few responses in, I gathered she was having the same conversation I’d had immediately after going active on the transplant list. When asked if I would donate my heart and lungs to science, I didn’t think twice. It’s still bizarre to me that researchers need permission to study the organs removed during a transplant. My friend agreed to sign the necessary forms to release her heart and lungs to the pathology lab, if and when she receives donor organs. Seems like a fair trade!
It’s not easy to decide to go on the transplant list, or to live without fear that you’ve either taken the plunge too soon or already waited too long. With several of my close friends going through transplant evaluation and listing processes, this weighs heavily on my mind.
After seeing my diseased heart and lungs outside my body, I never again questioned whether I made the right decision to have a transplant when I did. Nineteen days after my transplant, hospitalized with the last stubborn chest tube still draining, I got to visit Stanford’s aptly named Gross Room with my parents, my younger sister, my friend Carmela, a registered nurse, Nick (professional photographer), and my social worker.
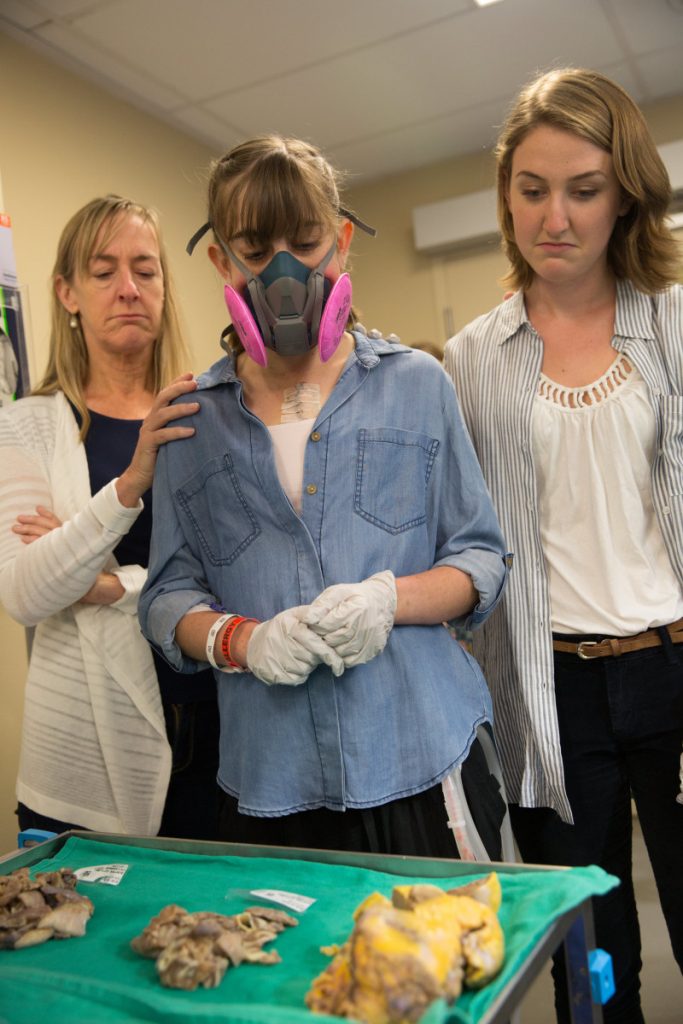
Nervous excitement mixed with shakiness from high doses of prednisone; I squeezed my sister’s hand for stability as we waited. My family put aside worries that had plagued us throughout the day, determined to honor the hard-working heart and lungs that took me as far as they could — an assertion solidified moments later.
A metal tray covered in green linen separated me from the pathologist assigned to introduce my newly outside insides. “That cloth isn’t fooling anyone,” I thought to myself and looked at him expectantly, wondering why he was waiting. The series of hallways and doors he’d guided us through had been enough of a grand reveal for me. Judging by the facial expressions Nick captured when the pathologist finally lifted the drape, it was indeed appropriate.
Three tidy piles rested before me. Yellowed by a layer of fat, what remained of my heart lay butchered beside conglomerates of gray lung tissue. Contrary to the cute analogies in my biology textbooks, my lungs were decidedly dissimilar to sponges. Riddled with calcium and fibrin deposits, the damage done by 23 years of pulmonary hypertension was refreshingly clear.
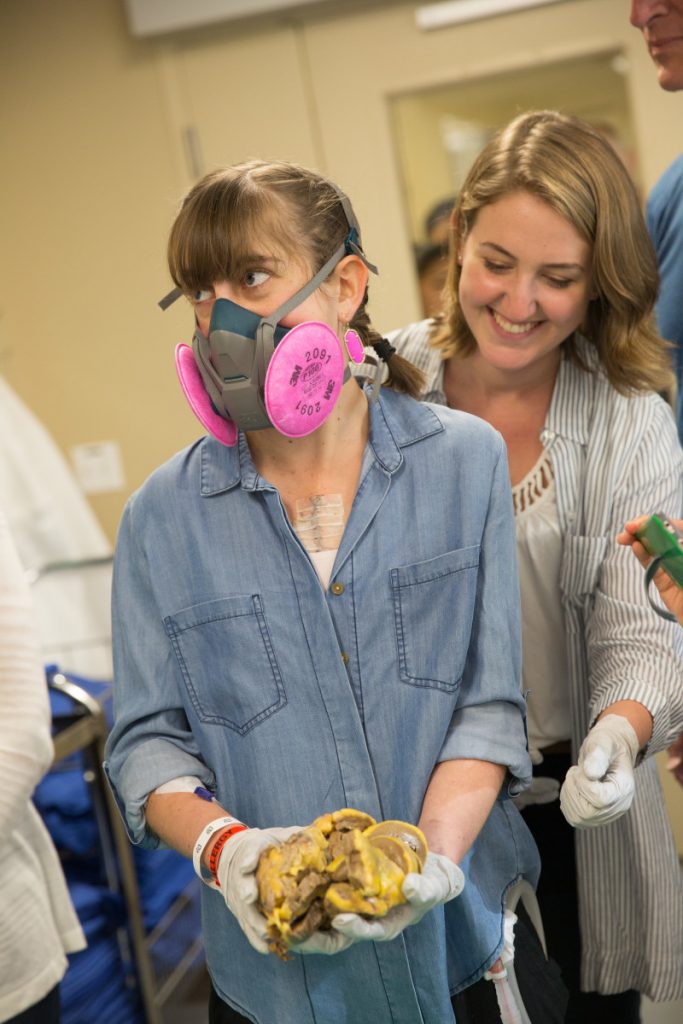
Chunks of abnormally thick heart wall fell back onto the cloth as I tried to piece together the mutilated remains into something resembling a human heart. “You’ve heard the words pulmonary hypertension,” the pathologist correctly presumed. Adrenaline coursed through my veins. I hadn’t completed a full eye roll before demanding he point out physical evidence of the Senning procedure I had at birth to correct transposition of the great arteries. “I’m gonna have a hard time with this, to be honest,” he confessed. My mask concealed my disappointment: not exactly the psyched-about-transposition expert I’d hoped for.
I pardoned his inability to locate the surgical intervention upon learning the wreckage before me lacked the atria where the intervention had occurred. That meant that the sections I held — one in each gloved hand, as if double-fisting grande caffè lattes — constituted only 60 percent of my tangled heart. My heart was massive: more than three times the appropriate size for my body.
During this visit, medications muddled my mind and inimitable pain exhausted my body. I felt bonded to the heart and lungs I was born with, and separating from them seemed unnatural. (It is.)
But seeing the trauma of my disease manifested in unmistakable physical form made me overwhelmingly happy to no longer have that heart and those lungs inside me and certain my transplanted organs had not come a moment too soon.
***
Note: Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Hypertension News or its parent company, Bionews Services, and are intended to spark discussion about issues pertaining to pulmonary hypertension.











Joanne
Wow, Kathleen! Thanks for sharing what must've been an almost indescribable moment. I had my pulmonary artery and valve replaced in January 2016 and beforehand, I arranged for them to be sent to a research university that's been studying my family's PH genetics. I prayed they might help researchers understand PH a little better. You are SO brave!!