Sarcoidosis and pulmonary hypertension
Pulmonary hypertension (PH) is a disorder characterized by high pressure in the vessels that carry blood from the heart to the lungs, called the pulmonary arteries. Among the potential causes of PH is the inflammatory disease sarcoidosis.
In sarcoidosis, masses of immune cells called granulomas form in various tissues throughout the body, leading to inflammation, scarring, and damage. When this occurs in or around the lungs, it can interfere with normal blood flow, leading to sarcoidosis-associated PH (SAPH).
SAPH belongs to Group 5 of the World Health Organization’s classification system for PH. Sarcoidosis is a rare cause of PH, but PH is a well-established complication of sarcoidosis. Around 5% to 28% of people with sarcoidosis may develop PH, which rises to 70% to80% in people with severe sarcoidosis lung complications or advanced disease.
SAPH is a serious condition that is associated with a worse prognosis for people with sarcoidosis. Therapeutic strategies vary on a case-by-case basis, but may include both sarcoidosis medications and PH treatment.
How sarcoidosis can cause pulmonary hypertension
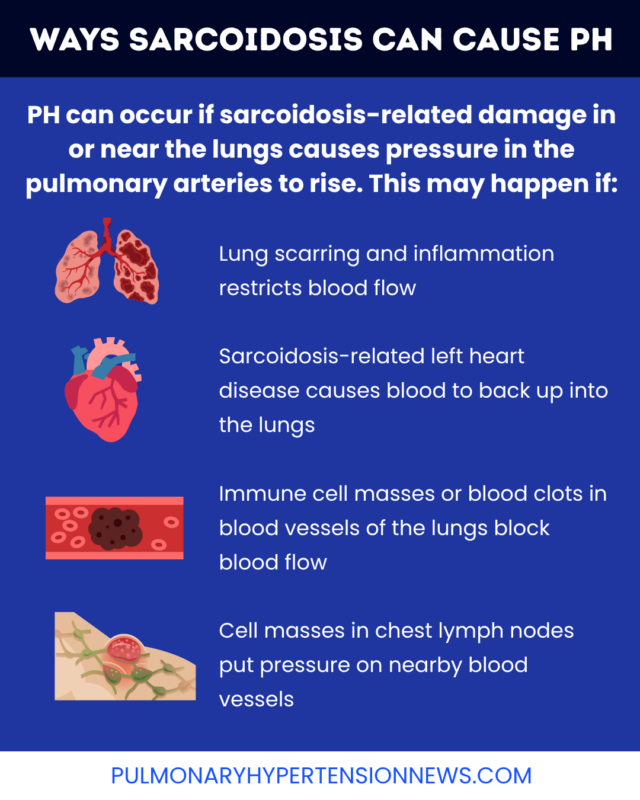
There are several ways in which sarcoidosis can increase pressure in the vessels around the lungs, called the pulmonary vasculature, contributing to PH. Such factors include:
- lung scarring and inflammation that damages blood vessels and may restrict blood flow
- sarcoidosis-related left heart disease that causes blood to back up into the lungs
- granulomas that form within the pulmonary vasculature and block blood flow
- blood clots in the pulmonary vasculature, which form more easily in people with sarcoidosis and can block blood flow
- granulomas that form in chest lymph nodes and put pressure on the pulmonary vasculature
Other possible symptoms of sarcoidosis, including sleep apnea, low oxygen transport through the bloodstream, and liver disease, may also put pressure on the heart and lungs.
Symptoms to watch for
If people with sarcoidosis start exhibiting PH symptoms, their doctor might run tests to look for SAPH. Such symptoms may include:
- shortness of breath
- chest pain
- heart palpitations
- fainting
- swelling
For some people with severe or advanced sarcoidosis, a doctor may recommend regular monitoring for signs of PH.
Diagnosis
If a person with sarcoidosis is showing signs of SAPH, their doctor will likely run a number of diagnostic tests to confirm the PH diagnosis, including:
- electrocardiograms and echocardiograms: noninvasive tests to assess heart structure and function
- pulmonary function and exercise tests: clinical examinations to evaluate lung function and exercise abilities
- imaging scans: X-rays, MRI, CT scans, or positron emission tomography (PET) to visualize abnormalities in the heart or lungs
- right heart catheterization (RHC): an invasive procedure that directly measures pulmonary artery pressure
While noninvasive tests can help screen for SAPH, RHC is ultimately required for a definitive diagnosis. This procedure involves threading a thin tube through a blood vessel and into the heart and pulmonary arteries to measure blood pressure. Because it is an invasive test, doctors may not perform it until other tests indicate that PH may be present.
In some cases, PH may be diagnosed first, and sarcoidosis later identified as the cause. If diagnostic tests show signs of granulomas, inflammation, and scarring, a doctor may establish sarcoidosis as the driver of PH.
Treatment and management options
Treating SAPH is an individualized process, and each patient will require a tailored management plan that accounts for disease mechanisms, PH severity, and other factors. In general, the process may involve:
- Treating the underlying sarcoidosis: Several treatments are available and aim to suppress the immune system. The most commonly used are corticosteroids, a class of powerful immunosuppressants.
- Supportive PH management: Supportive care can help manage PH symptoms. This may include oxygen therapy, which supplies extra oxygen to compensate for lung problems.
- PH-specific therapies: Several PH medications are available to help lower pulmonary artery pressure. However, none are specifically approved for SAPH in the U.S. Doctors might still recommend them in certain circumstances.
Other treatment strategies will depend on the mechanism by which sarcoidosis is causing PH. For example, if blood clots are obstructing the pulmonary vasculature, patients may undergo a procedure to remove the clots.
Some people with severe SAPH may require a lung transplant if other treatments don’t control symptoms.
Living with sarcoidosis and pulmonary hypertension
Like others living with PH, people with SAPH may need to adjust their daily habits to make disease management easier. For example, dietary changes and quitting smoking can help ease symptoms, and developing strategies to cope with PH fatigue can make participation in daily activities more feasible.
Exercise in PH can be challenging due to breathing difficulties and fatigue, though it is beneficial for overall health. Doctors can advise patients on the type of exercise suitable for them.
Emotional care is also important for people with SAPH and their caregivers. Support groups within the sarcoidosis or PH communities can offer patients both emotional and practical support in navigating life with these two rare conditions.
Pulmonary Hypertension News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
 Fact-checked by
Fact-checked by